Key Takeaways
- Standard ER X-rays image bone only — they routinely miss soft tissue injuries like ligament tears and cervical instability, which are among the most common crash injuries.
- MRI provides a static snapshot of soft tissue; DMX (Digital Motion X-Ray) captures how your cervical ligaments behave while moving — a critical distinction for detecting instability that MRI can miss.
- For Colorado personal injury claims, documentation that adheres to AMA guidelines matters. The imaging type you choose can directly affect how your injury is documented and understood by insurers and courts.
- This guide is for general educational purposes only. It does not replace individualized medical or legal advice. If symptoms are severe or worsening, seek urgent care immediately.
The short answer: X-rays show bones. MRIs show a static picture of soft tissue. Digital Motion X-Ray (DMX) shows how your cervical ligaments move — or fail to move correctly — in real time. If you left the ER after a crash with a “normal” X-ray but you’re still in pain, that result didn’t rule out a soft tissue injury. It simply wasn’t designed to find one.
Here’s what each imaging tool is actually built to detect, where each one falls short, and what Colorado injury documentation standards generally look for.
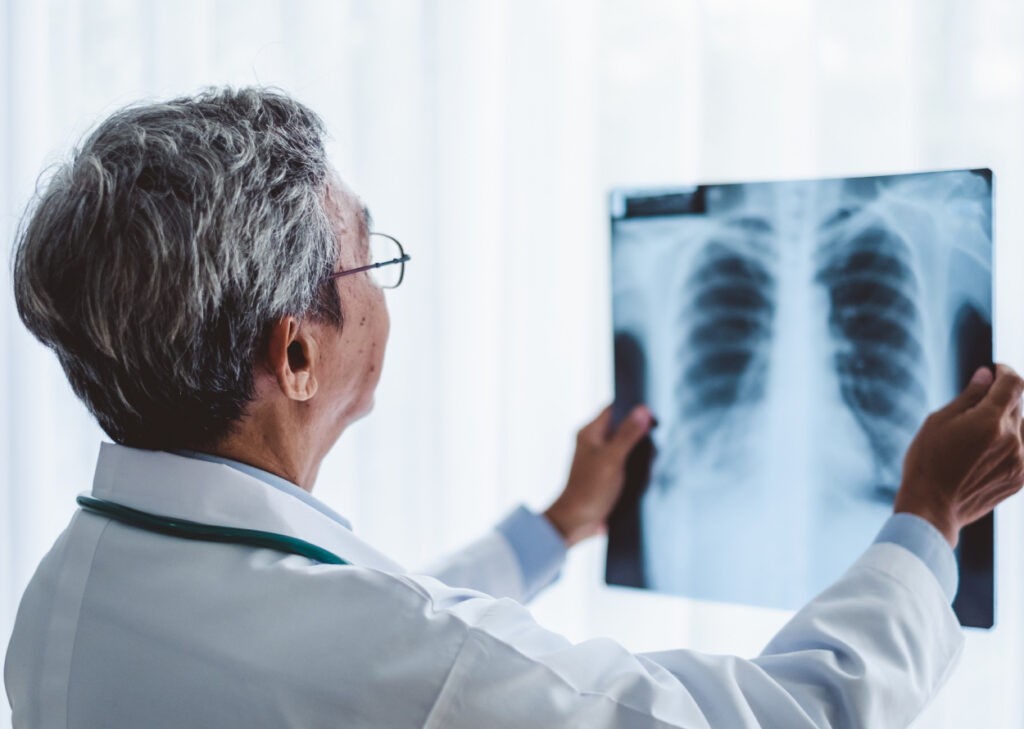
Why Your ER X-Ray Showed “Nothing Wrong” (And Why That’s Not the Whole Story)
After a rear-end collision on I-25 or a winter-weather crash on a Denver surface street, the ER’s first priority is ruling out fractures and life-threatening trauma. An X-ray is the right tool for that job.
But X-rays use ionizing radiation to produce images of dense structures — primarily bone. Ligaments, tendons, spinal discs, and the soft connective tissue of your cervical spine are largely invisible on a standard radiograph. A study published in the Journal of Orthopaedic Surgery and Research found that soft tissue injuries are present in a significant portion of whiplash patients whose initial X-rays appear completely normal.
This is not a failure of the ER. It’s a limitation of the technology. Your pain is real. The imaging just wasn’t designed to see it.
Seek urgent or emergency care if symptoms are severe, worsening, or include red-flag signs such as radiating arm pain, loss of coordination, or difficulty swallowing.
The Three Imaging Tools Compared — What Each One Actually Shows
X-Ray: The Baseline Bone Screener
Mechanism: Passes ionizing radiation through the body; dense structures (bone) absorb it and appear white on film.
What it shows well: Fractures, dislocations, bone spurs, gross spinal misalignment.
What it misses: Ligament tears, disc herniation, soft tissue inflammation, cervical instability, and the dynamic movement patterns that reveal ligament laxity.
Radiation exposure: Low to moderate (approximately 0.001–0.01 mSv for a cervical series). Generally considered safe in standard clinical use, though cumulative exposure is a consideration for repeat imaging.
Clinical role post-crash: Appropriate as an immediate triage tool. Not sufficient as a standalone diagnostic for Cervical Acceleration-Deceleration (Whiplash) injuries.
MRI: The Soft Tissue Snapshot
Mechanism: Uses magnetic fields and radio waves — no ionizing radiation — to produce detailed images of soft tissue structures.
What it shows well: Disc herniation, spinal cord compression, nerve root impingement, muscle tears, and some ligament injuries when swelling or tearing is significant enough to appear on a static image.
What it misses: Ligament laxity that only becomes apparent during movement. A ligament that is stretched or partially compromised may appear structurally intact on a static MRI, yet fail to stabilize the cervical spine under load or motion.
Contraindications: Standard MRI is contraindicated for patients with certain metallic implants, pacemakers, and some cochlear devices. Open MRI units exist as alternatives but typically offer lower image resolution.
Radiation exposure: None. MRI does not use ionizing radiation.
Clinical role post-crash: The most appropriate tool for evaluating disc pathology, nerve compression, and gross soft tissue injury. May not capture the full picture of cervical instability without complementary motion imaging.
Digital Motion X-Ray (DMX): The Ligament-in-Motion Test
Mechanism: A fluoroscopic technology that captures continuous, real-time X-ray video of the cervical spine during active movement. Rather than a single static frame, DMX produces a dynamic sequence showing how each vertebral segment moves relative to the others.
What it shows well: Abnormal intersegmental motion, ligament laxity, and cervical instability that only manifests under movement — the exact pathology that standard X-ray and static MRI can miss. This is why it is specifically referenced in AMA guidelines for documenting Cervical Acceleration-Deceleration injuries.
What it misses: DMX is not designed to evaluate disc herniation, nerve root compression, or soft tissue inflammation in the same detail as MRI. It is a motion-specific tool, not a replacement for MRI — it is a complement to it.
False-positive risk: A critical point that is often omitted by aggressive marketing: DMX requires a skilled, experienced clinician to interpret correctly. Artifacts, patient movement inconsistencies, and positioning variables can influence results. Findings should always be interpreted in the context of a full clinical evaluation, not in isolation.
Radiation exposure: Higher than a single static X-ray series due to the continuous fluoroscopic exposure. The clinical benefit must be weighed against radiation risk, particularly for younger patients, pregnant patients, and those requiring repeated imaging. A qualified provider will discuss this with you before ordering the study.
Contraindications: Pregnancy is a standard contraindication. Patients should disclose all relevant medical history before the study.
Clinical role post-crash: Most valuable when static imaging has been inconclusive, but clinical symptoms of cervical instability persist. Often ordered after an initial MRI and X-ray workup has been completed.
Side-by-Side Diagnostic Comparison Matrix
| X-Ray | MRI | DMX (Digital Motion X-Ray) | |
| Primary Use | Bone screening | Soft tissue & disc imaging | Cervical ligament motion analysis |
| Shows Fractures | Yes | Yes | Limited |
| Shows Disc Herniation | No | Yes | No |
| Shows Ligament Laxity | No | Partial (static only) | Yes (in motion) |
| Shows Cervical Instability | No | May miss dynamic cases | Yes |
| Radiation Exposure | Low–Moderate | None | Moderate (fluoroscopic) |
| AMA Whiplash Documentation | Baseline only | Supplementary | Specifically referenced |
| Contraindications | Pregnancy (limit) | Metal implants, pacemakers | Pregnancy |
| Cost Range (est.) | $100–$400 | $500–$3,000+ | $300–$1,500+ |
| Typically Covered by Colorado Med-Pay | Often | Often | Varies by policy |
Cost ranges are general estimates and vary by facility, provider, and insurance. Confirm coverage with your insurer.
Which Imaging Matters Most for a Colorado Personal Injury Claim?
This is where the clinical and legal realities intersect — and where the choice of imaging can have real consequences for how your injury is documented.
Colorado personal injury claims involving soft tissue injuries are frequently challenged by insurers precisely because standard X-rays appear normal. Comprehensive documentation that adheres to AMA guidelines — including objective findings from advanced imaging — can provide the clinical record that supports your case.
DMX findings, when interpreted by a qualified clinician and properly documented, are generally accepted as objective clinical evidence in Colorado personal injury proceedings. However, documentation standards matter. Imaging ordered and interpreted by a vetted, credentialed specialist carries significantly more weight than imaging from a facility unfamiliar with medico-legal documentation requirements.
To understand what specific documentation may be needed for your situation, connect with verified specialists who understand Colorado’s personal injury documentation standards and consult a qualified personal injury attorney. Documentation standards can matter in claims — talk to your provider and attorney about what’s appropriate for your specific case.
If you’re experiencing ongoing symptoms after a crash and want to understand your imaging options, our guide on delayed whiplash symptoms after a crash explains what to watch for in the days and weeks following a collision.
Does Colorado Med-Pay Cover Advanced Imaging Like MRI or DMX?
Colorado law requires auto insurance policies to offer Medical Payments (Med-Pay) coverage, which may help cover reasonable and necessary medical expenses — including diagnostic imaging — regardless of fault. However, coverage varies significantly by policy.
MRI is typically considered a standard diagnostic procedure and is more commonly covered under Med-Pay without prior authorization. DMX, as a specialized fluoroscopic study, may require documentation of medical necessity and prior authorization depending on your insurer and policy terms.
What this means practically: Before scheduling advanced imaging, ask your provider to document the clinical necessity clearly in your records. A vetted specialist familiar with Colorado Med-Pay laws and navigating insurance for advanced diagnostics can help ensure the imaging is ordered and documented in a way that supports your coverage request.
Colorado Med-Pay may help cover eligible medical expenses depending on your policy. Coverage varies — confirm specifics with your insurance provider.
Frequently Asked Questions
Does an MRI show ligament damage from whiplash?
MRI can detect significant ligament tears when there is enough structural disruption to appear on a static image. However, ligament laxity — where a ligament is stretched or partially compromised but not fully torn — may not be visible on a standard MRI. In these cases, dynamic motion imaging such as DMX may provide additional clinical information that a static MRI cannot. A licensed clinician can evaluate which imaging is appropriate based on your specific symptoms and clinical presentation.
Is Digital Motion X-Ray (DMX) safe after a car accident?
DMX uses fluoroscopic X-ray technology, which does involve ionizing radiation exposure — more than a single static X-ray series due to its continuous nature. For most adults, the clinical benefit of diagnosing cervical instability is considered to outweigh the radiation risk when ordered appropriately. DMX is generally contraindicated during pregnancy. Patients with specific health conditions should discuss the risks and benefits with their ordering clinician before proceeding. A qualified provider will review your history before recommending the study.
Do I need imaging before I can file a personal injury claim in Colorado?
There is no legal requirement to obtain specific imaging before filing a claim. However, objective clinical findings — including imaging results — can play an important role in documenting the nature and extent of your injuries. Claims involving only subjective pain reports and no objective imaging are more frequently disputed by insurers. For guidance on what documentation may be appropriate for your specific situation, consult a qualified personal injury attorney and a clinician experienced in objective findings for personal injury claims.
What to Do Next
If you left the ER with a “normal” X-ray but you’re still experiencing neck pain, headaches, brain fog, or radiating symptoms, your injury may simply not have been visible on the imaging used.
Understanding which diagnostic tool is right for your situation is a clinical decision that should involve a licensed professional who understands both the biomechanics of crash injuries and the documentation standards that matter in Colorado.
Connect with verified specialists in the Colorado Car Accident Chiropractor network — every provider is vetted for credentials, board certifications, and experience with advanced diagnostics, including DMX and MRI for Cervical Acceleration-Deceleration injuries.
This page provides general educational information and does not provide medical, legal, or insurance advice. For guidance specific to your situation, consult a licensed healthcare professional and/or qualified attorney, and confirm coverage details with your insurance provider. If symptoms are severe, worsening, or you are concerned about a head or neck injury, seek urgent or emergency care.
 Concussion vs. Whiplash Overlap: What to Monitor After a Car Accident
Concussion vs. Whiplash Overlap: What to Monitor After a Car Accident