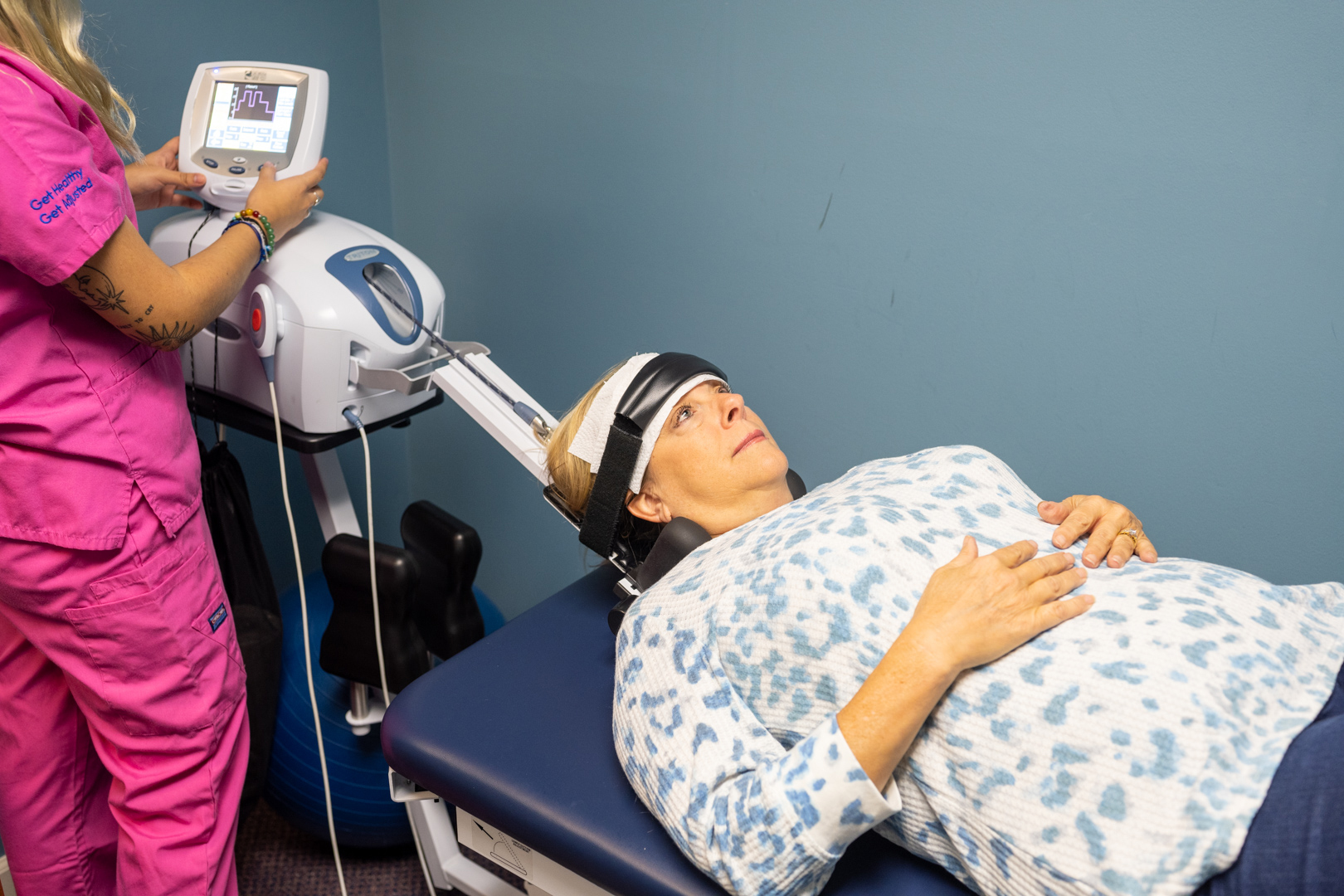
Spinal Decompression Therapy
Spinal Decompression Therapy: A Clinical Guide to Non-Surgical Disc Recovery in Colorado
Spinal decompression therapy is a non-surgical treatment protocol that uses controlled, computerized traction to create negative intradiscal pressure within the vertebral discs. This negative pressure (typically -150 mmHg) promotes a vacuum effect called imbibition, which draws oxygen, nutrients, and hydration back into damaged discs while reducing pressure on compressed nerve roots. Unlike manual traction, modern decompression systems use biofeedback sensors to detect and bypass muscle guarding—a critical distinction for trauma patients whose nervous systems remain in a protective state following high-velocity injuries such as car accidents.
The distinction between therapeutic decompression and standard traction lies in the sophistication of force application. While traditional traction applies continuous linear force that often triggers protective muscle spasms, computerized decompression uses logarithmic force curves that incrementally increase tension over precise intervals. This gradual progression, monitored by real-time biofeedback, prevents the body’s natural guarding response and allows the disc to experience true decompression rather than simply stretching surrounding soft tissue.
Table of Contents[Hide][Show]
- How Computerized Spinal Decompression Works: The Mechanism of Action
- The “Muscle Guarding” Problem: Why Standard Traction Often Fails
- Clinical Applications: Conditions Treated with Decompression Therapy
- Technology Comparison: DRX9000, SpineMED, and FDA-Cleared Devices
- Treatment Protocols and Expected Timelines
- Frequently Asked Questions About Spinal Decompression
Comprehensive Recovery Treatments for Colorado Auto Injury Patients
If you’re experiencing persistent pain following a car accident, spinal decompression may be part of a broader recovery protocol tailored to trauma patients. Colorado auto injury specialists often integrate multiple evidence-based therapies to address both immediate symptoms and long-term tissue healing:

Complete Post-Crash Recovery Protocols – Comprehensive assessment and treatment planning for accident-related injuries

Accelerate Soft Tissue Healing with Class IV Laser – Photobiomodulation therapy to reduce inflammation and promote cellular regeneration

Targeted Relief for Radiating Leg Pain – Specialized protocols for sciatic nerve compression and lower extremity radiculopathy

Spinal Alignment and Joint Mobilization – Precise adjustments to restore proper vertebral mechanics
Deep Tissue Muscle Release Therapy – Mechanical vibration therapy to address trigger points and fascial adhesions
Each of these treatments addresses different layers of trauma recovery, and your provider will determine which combination is appropriate based on diagnostic findings and injury severity.
Find a Spinal Decompression Therapy Specialist Near You
The Physiology of Disc Compression Following Trauma
The human spine is engineered to withstand vertical loading forces during normal daily activities, but it’s particularly vulnerable to horizontal acceleration-deceleration forces common in vehicle collisions. During a rear-end impact, occupants experience forces ranging from 2.5 to 5 Gs depending on collision speed. These forces compress the intervertebral discs anteriorly while stretching posterior ligaments and soft tissue structures.
The intervertebral disc consists of two distinct components: the nucleus pulposus (a gel-like center composed of approximately 80% water in healthy discs) and the annulus fibrosus (concentric rings of fibrocartilage that contain the nucleus). When traumatic compression occurs, the nucleus can migrate posteriorly or posterolaterally, creating a bulge or herniation that encroaches on the spinal canal or intervertebral foramen. This mechanical compression of nerve roots produces the characteristic radiating pain known as radiculopathy.
What distinguishes trauma-induced disc injury from degenerative disc disease is the acute nature of the damage and the accompanying ligament laxity. In whiplash injuries, the anterior longitudinal ligament and the disc-vertebral junction can become compromised, reducing the spine’s ability to maintain proper spacing between vertebrae. Standard imaging (static X-rays or MRI) may show disc pathology but often fails to capture the dynamic instability that perpetuates symptoms. This is why advanced diagnostic tools like Digital Motion X-Ray (DMX) are valuable for diagnosing hidden ligament instability in trauma cases.
The body’s inflammatory response to disc injury further complicates healing. Chemical irritants from the damaged nucleus (including phospholipase A2 and other inflammatory mediators) can leak into surrounding tissue, creating pain that’s disproportionate to the mechanical compression alone. This biochemical component of disc pain explains why purely mechanical interventions like traditional traction sometimes provide incomplete relief.
How Computerized Spinal Decompression Works: The Mechanism of Action
The therapeutic goal of spinal decompression is to reverse intradiscal pressure from positive (compressive) to negative (decompressive), creating an environment where the disc can rehydrate and retract herniated material. Research using pressure transducers inserted directly into cadaveric discs has confirmed that properly calibrated decompression can achieve negative intradiscal pressures of -150 to -200 mmHg.
This negative pressure creates a vacuum effect within the disc space, which triggers imbibition—the process by which water, oxygen, and nutrients from surrounding capillaries are drawn into the disc through osmotic pressure. Healthy discs undergo imbibition naturally during rest and sleep when spinal loading decreases. However, in acutely injured or chronically degenerated discs, this process becomes impaired. Decompression therapy essentially amplifies and accelerates this natural healing mechanism.
The treatment protocol typically positions the patient on a specialized table with a harness system that targets either the lumbar spine (lower back) or cervical spine (neck). The computerized system then applies distraction force in a precise, pre-programmed pattern. Rather than sustaining constant tension, the machine cycles between distraction and partial relaxation phases, typically holding peak tension for 30-60 seconds before briefly releasing.
This cycling pattern serves two critical purposes. First, it prevents the body’s mechanoreceptors from adapting to a sustained stretch, which would diminish the therapeutic effect over time. Second, it creates a pumping action that enhances fluid exchange within the disc—drawing in nutrients during the distraction phase and flushing out metabolic waste during the partial release phase.
The angle of distraction is also strategically determined based on the specific disc level being targeted. For lower lumbar segments (L4-L5, L5-S1), the table may be positioned to create slight hip flexion, which opens the posterior disc space where most herniations occur. For cervical treatments addressing whiplash injuries at C5-C6 or C6-C7, the angle of pull is calculated to decompress the specific compromised segment while maintaining the cervical lordosis (natural forward curve of the neck).
The “Muscle Guarding” Problem: Why Standard Traction Often Fails
The single greatest challenge in treating trauma patients with manual traction is the phenomenon of muscle guarding, also called the proprioceptor reflex. When the body perceives a pulling force on the spine, specialized nerve receptors in the muscles and ligaments (particularly the muscle spindles and Golgi tendon organs) send rapid signals to the spinal cord, triggering an immediate protective contraction of the paraspinal muscles.
This protective response evolved to prevent tissue damage from excessive stretching, but in the clinical setting, it sabotages the therapeutic goal. When paravertebral muscles contract against the traction force, the actual tension reaching the disc is significantly reduced—sometimes by 50% or more. The patient is pulled, but the disc itself never experiences meaningful decompression. This explains why patients often report that traditional traction “felt good during the session” but provided only temporary relief.
Computerized decompression systems solve this problem through real-time biofeedback monitoring. Sensors embedded in the harness or table continuously measure resistance. When the system detects an increase in resistance indicating muscle contraction, it responds in milliseconds by slightly reducing tension. This reduction occurs so quickly (often within 20-50 milliseconds) that the patient is typically unaware of the adjustment. The proprioceptor response is essentially bypassed before it can fully develop.
This logarithmic force application—gradual increases interrupted by micro-pauses and adjustments—is fundamentally different from the linear force curve of manual traction. Studies comparing standard traction to computerized decompression have found that decompression achieves significantly greater vertebral separation (measured via fluoroscopy) and produces negative intradiscal pressure, while traction often fails to move the pressure below zero.
For post-trauma patients, this distinction is especially critical. Following a car accident, the nervous system remains in a heightened protective state—a phenomenon sometimes called central sensitization. These patients exhibit exaggerated muscle guarding responses compared to individuals with degenerative pain. A treatment approach that can work around this protective barrier is essential for achieving therapeutic outcomes in the trauma population.
Clinical Applications: Conditions Treated with Decompression Therapy
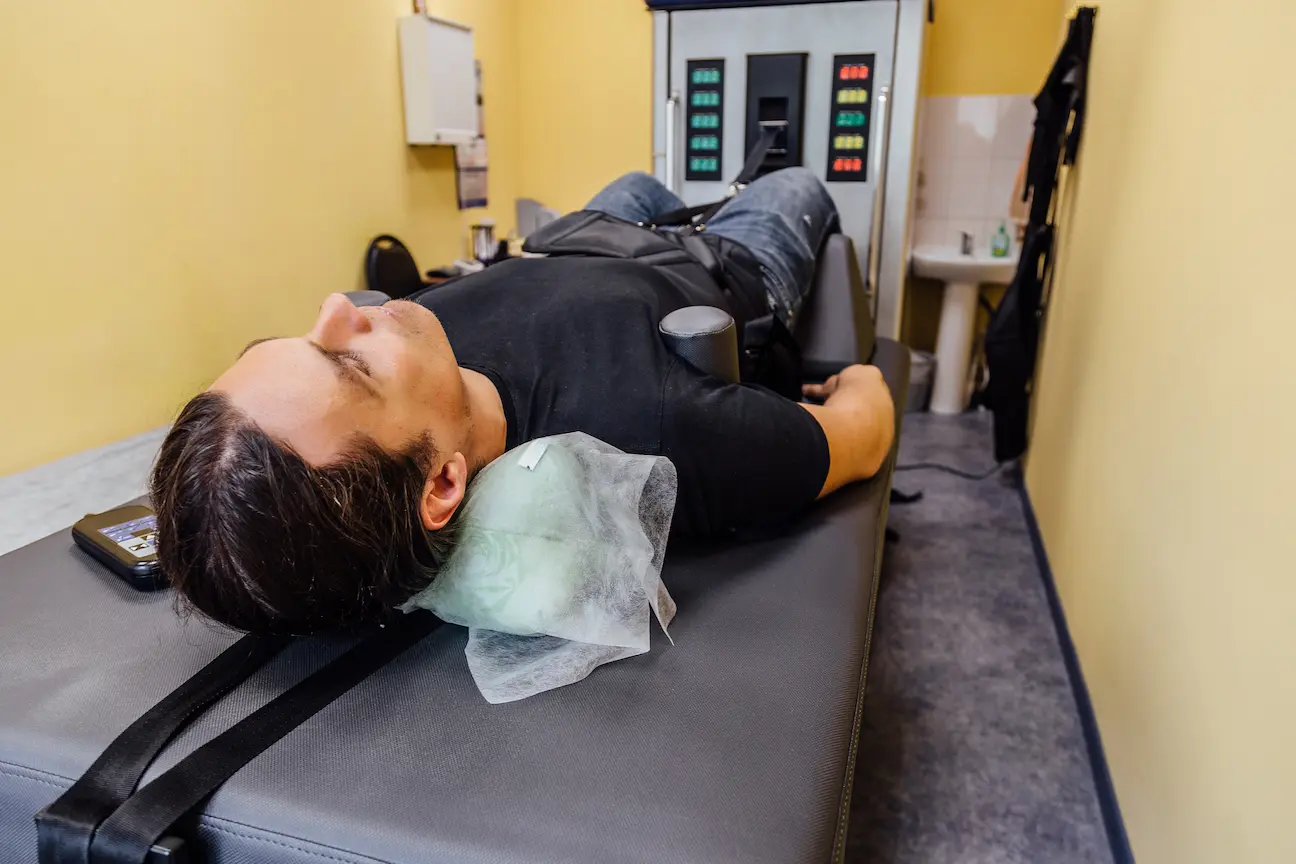
Spinal decompression therapy has demonstrated clinical effectiveness for several specific conditions, particularly those involving mechanical nerve compression and disc pathology:
Herniated and Bulging Discs: When the annulus fibrosus tears or weakens, allowing the nucleus pulposus to protrude beyond the normal disc margin, decompression can help retract the herniated material through negative pressure. Retraction of even 1-2 millimeters can significantly reduce nerve root compression and alleviate radiating pain.
Radiculopathy (Nerve Root Compression): Whether cervical radiculopathy causing arm pain, numbness, and weakness, or lumbar radiculopathy producing sciatica, decompression addresses the mechanical component by increasing intervertebral space and reducing nerve impingement. This is particularly effective when radiculopathy is caused by disc herniation rather than bony stenosis.
Post-Whiplash Syndrome: Cervical acceleration-deceleration injuries often produce multi-level disc injuries and ligament laxity that don’t respond to conservative chiropractic adjustments alone. Decompression can address the disc component while other therapies (laser, percussor therapy) address soft tissue damage.
Failed Conservative Treatment: Patients who have undergone weeks or months of standard physical therapy, chiropractic care, or epidural injections without resolution often respond to decompression because it addresses the mechanical disc problem more directly than these other approaches.
Degenerative Disc Disease with Acute Exacerbation: While decompression cannot reverse long-term degeneration, it can provide significant relief during acute flare-ups by rehydrating discs and reducing inflammatory pressure on adjacent structures.
Facet Syndrome: Though primarily a disc therapy, decompression also reduces stress on facet joints by restoring disc height, which can alleviate pain from facet inflammation or capsular irritation.
Contraindications do exist and must be carefully screened during evaluation. These include pregnancy, severe osteoporosis, spinal tumors, fractures, abdominal aortic aneurysm, and certain types of spinal hardware. Patients who have undergone fusion surgery generally cannot receive decompression at the fused segment, though adjacent levels may sometimes be treated. A thorough examination including imaging review is essential to determine candidacy.
Technology Comparison: DRX9000, SpineMED, and FDA-Cleared Devices
The term “spinal decompression” has unfortunately been applied to a wide range of devices with vastly different capabilities. Understanding the distinction between true decompression systems and simple traction tables is important when evaluating treatment options.
FDA-Cleared Computerized Decompression Systems include brands such as the DRX9000, SpineMED, VAX-D, and Triton DTS. These systems share several critical features: computerized force control, biofeedback sensors to monitor muscle resistance, programmable logarithmic force curves, and the ability to target specific spinal segments through angle adjustment. Most are classified as FDA Class II medical devices, meaning they’ve undergone regulatory review for safety and performance claims.
The DRX9000 was one of the first widely adopted systems and remains popular in many clinics. It features a split table design that allows the lower section to move independently, and its software includes pre-set protocols for different conditions. The system can apply distraction forces up to 350 pounds for lumbar treatment, with force ramping up in gentle increments over several minutes.
SpineMED systems emphasize patient comfort and control, featuring a prominent patient safety switch that allows immediate release of tension if discomfort occurs. The biofeedback system is particularly sensitive, making micro-adjustments throughout the treatment cycle. Some practitioners prefer SpineMED for treating anxious patients or those with high levels of central sensitization.
Inversion Tables and Home Traction Units, while sometimes marketed as “decompression,” do not provide true therapeutic decompression. Inversion relies on body weight and gravity, producing uncontrolled and non-specific force that cannot be targeted to individual disc levels. Home traction units lack biofeedback systems and cannot overcome muscle guarding. While these devices may provide temporary symptomatic relief for some users, they should not be confused with clinical decompression therapy.
Safety Features are paramount in professional decompression systems. Most include emergency stop buttons accessible to both patient and provider, automatic pause functions if excessive resistance is detected, and maximum force limits that prevent over-distraction. The patient remains fully clothed and is positioned comfortably for the 20-30 minute session. Many patients report feeling significant relief during the treatment itself, and some even fall asleep due to the rhythmic stretching and relaxation.
Clinics using advanced imaging—such as pre- and post-treatment MRI or fluoroscopy—can sometimes document objective changes in disc morphology, including reduction in herniation size or increased disc height. This objective documentation is particularly valuable for patients pursuing personal injury claims following auto accidents, as it provides quantifiable evidence of injury severity and treatment response.
Treatment Protocols and Expected Timelines
A typical spinal decompression protocol for trauma patients consists of 20-30 sessions over 6-8 weeks, though the exact duration depends on injury severity, chronicity, and individual response. Initial treatments are usually scheduled 3-4 times per week during the acute phase, then tapered to 2-3 times weekly as symptoms improve.
Each individual session lasts approximately 20-30 minutes of decompression time, with additional time for positioning and post-treatment therapies. Many protocols combine decompression with complementary modalities in the same visit—for example, 25 minutes of decompression followed by 10 minutes of Class IV laser therapy to accelerate soft tissue healing and reduce inflammation.
Phase 1 (Weeks 1-3): Acute Symptom Reduction
The initial phase focuses on reducing pain and inflammation. Patients often report decreased radiating symptoms within the first 6-10 sessions as disc pressure is relieved and nerve root compression diminishes. During this phase, patients are typically advised to avoid heavy lifting, prolonged sitting, and activities that increase intradiscal pressure (forward bending, twisting).
Phase 2 (Weeks 4-6): Tissue Healing and Stabilization
As acute symptoms subside, the focus shifts to disc rehydration and healing. The imbibition process continues with each session, gradually improving disc integrity. Many protocols introduce gentle rehabilitation exercises during this phase to begin restoring core strength and spinal stability. The exercises are carefully selected to avoid compromising the healing disc while building the muscular support needed for long-term success.
Phase 3 (Weeks 7-8+): Maintenance and Transition
The final phase reduces treatment frequency to allow the body to maintain improvements independently. Some protocols incorporate “maintenance” sessions (1-2 per month) for patients at high risk of re-injury or those with significant degenerative changes. Patients are transitioned to a home exercise program emphasizing core stabilization, proper ergonomics, and lifestyle modifications.
Response Indicators: Clinical outcomes are monitored through objective measures including pain scale ratings (VAS or numeric rating scale), functional assessments (Oswestry Disability Index for lumbar conditions, Neck Disability Index for cervical conditions), orthopedic testing (straight leg raise, Kemp’s test), and neurological examination (reflexes, sensation, motor strength). Patients who show minimal improvement after 12-15 sessions may require re-evaluation, including possible advanced imaging to rule out complicating factors.
Research on clinical outcomes varies by condition, but studies generally report that 70-85% of patients with herniated discs experience significant improvement, while success rates for degenerative conditions are somewhat lower but still meaningful. Trauma patients with documented ligament laxity and multi-level involvement may require longer protocols and often benefit from concurrent therapies such as prolotherapy or platelet-rich plasma (PRP) to address ligamentous healing.
Colorado-Specific Considerations: Med-Pay and Medical Documentation

Understanding insurance coverage is crucial for Colorado auto accident victims considering spinal decompression therapy. Many patients are unaware that Colorado law requires all auto insurance policies to include Medical Payments Coverage (Med-Pay) unless explicitly rejected in writing by the policyholder.
Colorado Med-Pay Explained: Med-Pay is “no-fault” coverage that pays for medical expenses related to auto accidents regardless of who caused the collision. Coverage amounts typically range from $5,000 to $50,000, though $5,000 is the state-required minimum. Unlike standard health insurance, Med-Pay generally has no deductible and no copayment—it covers 100% of approved medical treatment up to the policy limit.
For spinal decompression therapy, which can cost $2,000-$5,000 for a complete protocol, Med-Pay provides critical access to treatment without out-of-pocket expense. The key requirement is that treatment must be “reasonable and necessary” as a result of the accident, and care should begin within a reasonable timeframe (ideally within weeks of the collision, though exceptions exist for delayed-onset symptoms).
Documentation Standards for Legal Claims: Colorado auto injury cases often involve personal injury claims against at-fault drivers. The quality of medical documentation directly impacts settlement value and litigation success. Providers specializing in trauma care understand the importance of thorough documentation following the AMA Guides to the Evaluation of Permanent Impairment.
Critical documentation elements include:
- Initial examination findings with objective orthopedic and neurological testing
- Diagnostic imaging reports (X-ray, MRI) with specific findings regarding disc pathology
- Causation statements linking the documented injuries to the specific accident
- Treatment records detailing each therapy session and the patient’s response
- Progress evaluations showing objective improvement or plateau
- Impairment ratings if permanent restrictions result
Advanced diagnostics such as Digital Motion X-Ray (DMX) can be particularly valuable for documenting ligament laxity and segmental instability that don’t appear on static imaging. This technology captures real-time movement of the cervical spine through flexion and extension, revealing excessive translation or angular motion that indicates ligament damage.
Working with Attorneys: Many Colorado auto injury patients are represented by personal injury attorneys. Reputable medical providers maintain professional relationships with the legal community while maintaining clinical independence. Some clinics offer lien-based treatment for patients whose Med-Pay has been exhausted but who have viable third-party claims. This arrangement allows treatment to continue with payment deferred until the case settles, though patients should understand the terms and risks of lien agreements before proceeding.
Providers certified in Whiplash and Brain Injury Traumatology bring specialized knowledge of crash biomechanics and injury patterns that strengthens medical testimony if a case proceeds to litigation or arbitration. This certification demonstrates commitment to evidence-based trauma care beyond general chiropractic or physical therapy practice.
Decompression Therapy vs. Other Interventions
Patients exploring treatment options for disc injuries often face confusion about how different approaches compare. The following comparison clarifies the role of decompression relative to other common interventions:
| Treatment | Mechanism | Best For | Limitations |
| Computerized Decompression | Negative intradiscal pressure via biofeedback-controlled traction | Herniated discs, radiculopathy, failed conservative care | Requires multiple sessions; not suitable for fractures, severe instability, or certain hardware |
| Standard Traction | Sustained linear pulling force | Mild muscle spasm, general stiffness | Cannot overcome muscle guarding; doesn’t achieve negative disc pressure |
| Chiropractic Adjustments | High-velocity, low-amplitude thrust to restore joint motion | Facet restrictions, acute subluxations, mild disc bulges | May aggravate large herniations; doesn’t address disc hydration |
| Epidural Steroid Injections | Anti-inflammatory medication delivered to epidural space | Severe acute inflammation, radicular pain | Temporary relief (weeks to months); doesn’t address mechanical problem; carries infection/nerve damage risks |
| Physical Therapy | Exercise, manual therapy, modalities | Muscle weakness, post-surgical rehab, chronic pain | Limited effectiveness for acute disc herniation without addressing mechanical compression |
| Surgical Discectomy | Removal of herniated disc material | Severe neurological compromise, cauda equina syndrome, failed conservative care | Invasive; recovery time; doesn’t prevent recurrence; risk of failed back surgery syndrome |
The ideal approach for many trauma patients involves a multimodal protocol that addresses different components of injury. Decompression handles the mechanical disc problem, Class IV laser reduces inflammation and accelerates tissue healing at the cellular level, chiropractic adjustments restore proper segmental motion, and rehabilitative exercise rebuilds strength and stability.
Patients with “failed back surgery syndrome”—persistent or recurrent pain following discectomy or fusion—sometimes pursue decompression for adjacent segments that have degenerated due to altered biomechanics. While these cases are more complex and require careful evaluation, non-surgical options should be explored before considering revision surgery.
Frequently Asked Questions About Spinal Decompression
What is the difference between spinal decompression and standard traction?
Standard traction applies a continuous pulling force using weights or manual tension. This linear force often triggers a protective muscle spasm called guarding, which reduces the actual tension reaching the disc. Computerized spinal decompression uses biofeedback sensors that detect muscle resistance in real-time and adjust the force application in milliseconds. The result is a logarithmic force curve that bypasses the guarding reflex, allowing the disc to experience true negative pressure. Clinical studies using pressure transducers have confirmed that decompression achieves negative intradiscal pressures of -150 mmHg or lower, while standard traction typically fails to bring pressure below zero. This distinction is critical for achieving therapeutic outcomes in trauma patients whose nervous systems remain in a heightened protective state.
How many sessions are typically required to see permanent results?
Most clinical protocols for disc injuries involve 20-30 sessions over 6-8 weeks, though individual response varies based on injury severity, chronicity, and complicating factors. Many patients report noticeable symptom reduction within the first 8-12 sessions as nerve root compression decreases. However, tissue healing—particularly rehydration of the disc through imbibition—requires sustained treatment over weeks. The term “permanent” requires clarification: decompression can produce lasting improvement in disc integrity and symptom relief, but it doesn’t prevent future injury or age-related degeneration. Patients who maintain core strength, practice proper ergonomics, and avoid high-risk activities tend to sustain their improvements long-term. Some individuals with significant degenerative changes may benefit from periodic maintenance sessions (monthly or quarterly) to preserve disc health.
Is spinal decompression therapy covered by major medical insurance or Medicare?
Coverage varies significantly by insurance carrier and policy type. Traditional health insurance plans (Blue Cross, United Healthcare, Aetna, etc.) may cover decompression when it’s deemed medically necessary and prescribed by a physician, though many plans categorize it as “experimental” or limit the number of covered sessions. Pre-authorization is often required. Medicare does not typically cover spinal decompression therapy directly, though related services (evaluation, X-rays) may be covered. The most favorable coverage scenario for Colorado patients is auto accident injuries where Medical Payments Coverage (Med-Pay) applies. Because Med-Pay is “no-fault” coverage required under Colorado law, it generally covers spinal decompression 100% without copays or deductibles as long as treatment is reasonable and necessary. Patients should verify their specific Med-Pay limit and work with providers who have experience navigating auto injury insurance claims.
Can spinal decompression help if I have already had back surgery?
This depends on the type of surgery and the specific problem being addressed. Patients who have undergone surgical fusion cannot receive decompression at the fused segment because those vertebrae are permanently locked together. However, decompression can sometimes be applied to adjacent levels that have developed problems due to altered biomechanics (a condition called “adjacent segment disease”). Patients who had a discectomy or laminectomy without fusion may be candidates for decompression if residual or recurrent symptoms arise, though careful evaluation is essential to rule out complications such as recurrent herniation or scarring (epidural fibrosis). Patients with certain types of spinal hardware (rods, screws, plates) may be contraindicated depending on the location and stability of the instrumentation. If you’re experiencing “failed back surgery syndrome,” consult with a provider experienced in post-surgical cases who can perform a thorough examination and review your surgical records before making a recommendation.
What are the specific contraindications or risks associated with decompression therapy?
Absolute contraindications include pregnancy (due to harness pressure on the abdomen), severe osteoporosis (risk of fracture under tension), spinal tumors or infections, abdominal aortic aneurysm (risk of rupture), and acute spinal fractures. Relative contraindications requiring careful evaluation include spinal fusion at the target segment, certain types of hardware, extreme spinal instability, and patients taking anticoagulants (blood thinners) who may be at increased bleeding risk. Adverse effects are generally rare and mild when contraindications are properly screened. Some patients experience temporary soreness similar to post-exercise muscle fatigue, which typically resolves within 24 hours. In very rare cases, patients may experience increased pain if the treatment force is too aggressive or if underlying pathology was not properly identified. This is why thorough examination including imaging review is essential before beginning treatment. Properly administered decompression by a qualified provider has a strong safety record with significantly fewer risks than surgical intervention or long-term opioid use.
How does the machine know how much force to apply to the spine?
Modern decompression systems use sophisticated computer programming combined with real-time biofeedback monitoring. Before treatment begins, the provider inputs patient-specific parameters including body weight, disc level being targeted, and treatment phase (initial vs. advanced). The system then calculates an appropriate maximum force—typically 50-60% of body weight for lumbar treatment, less for cervical treatment. During the session, sensors in the harness or table continuously measure resistance. When the computer detects an increase in resistance indicating muscle contraction, it responds by slightly reducing tension, then gradually reapplying force once the muscles relax. This creates a logarithmic curve where force increases in incremental steps with micro-pauses, rather than a linear ramp-up. The provider can adjust protocols session by session based on patient response, gradually increasing maximum force as tolerance improves. Most systems also feature patient safety controls—a large button that allows the patient to immediately release all tension if discomfort occurs. This combination of computerized precision and patient control ensures safe, individualized treatment.
Is the treatment painful for patients with acute sciatica?
Most patients with acute sciatica report that decompression provides relief rather than causing pain. The gentle, gradual application of force typically does not aggravate symptoms, and many patients notice decreased radiating leg pain during the session itself as nerve root pressure is temporarily reduced. However, initial sessions may produce mild soreness in the low back muscles (similar to a stretching workout) as tissue adapts to the mechanical force. This soreness is distinct from nerve pain and generally diminishes after the first 3-4 treatments. In rare cases, if a disc herniation is extremely large or if the patient has severe central canal stenosis (narrowing), certain movements or positions may initially aggravate symptoms. This is why proper positioning and angle adjustment are critical. Providers experienced in treating trauma patients will start conservatively with lower force settings and gradually progress as tolerance improves. If pain significantly worsens during treatment, the session should be stopped and the clinical picture re-evaluated. Overall, the treatment is designed to reduce pain, and proper patient selection and technique make it well-tolerated even for those with acute, severe symptoms.