
Laser Therapy
Laser Therapy for Tissue Repair: A Complete Guide to Photobiomodulation Science & Clinical Applications
Laser therapy, clinically known as photobiomodulation (PBM), is an FDA-cleared treatment that uses specific wavelengths of light (600-1000nm) to stimulate cellular repair in damaged soft tissues. By triggering ATP production in mitochondria and increasing local blood flow, laser therapy accelerates the body’s natural healing response for conditions ranging from acute whiplash injuries to chronic neuropathic pain. Unlike pharmaceutical interventions that mask symptoms, photobiomodulation works at the cellular level to support the body’s inherent repair mechanisms.
Table of Contents[Hide][Show]
Safety Profile: Contraindications, Side Effects & Device Clearance+−
- FDA Clearance Status
- Contraindications (When Not to Use Laser Therapy)
- Safety with Medical Devices
- Side Effects
- The Medico-Legal Documentation Advantage: Colorado Auto Injury Claims
- The “Soft Tissue Injury” Problem
- AMA Guidelines and Objective Treatment Records
- Colorado Med-Pay Coverage
- Lien-Based Treatment
- Frequently Asked Questions About Laser Therapy
Need Specialized Treatment for Your Specific Condition?
Laser therapy protocols are most effective when integrated with targeted rehabilitation for your specific injury type. Our Colorado clinics combine advanced photobiomodulation with specialized care approaches:

Whiplash & Post-Crash Soft Tissue Recovery – Comprehensive protocols for cervical acceleration-deceleration injuries
Nerve Compression & Radiating Pain – Specialized care for sciatica and radiculopathy
Disc Herniation & Decompression – Non-surgical disc treatment combining laser therapy with mechanical decompression
Joint Mobilization & Spinal Alignment – Manual therapy enhanced by tissue preparation with laser treatment
Deep Muscle Trigger Point Release – Mechanical percussion therapy for adhesions and fascial restrictions
Find a Laser Therapy Specialist Near You
Understanding Photobiomodulation: How Light Triggers Cellular Repair
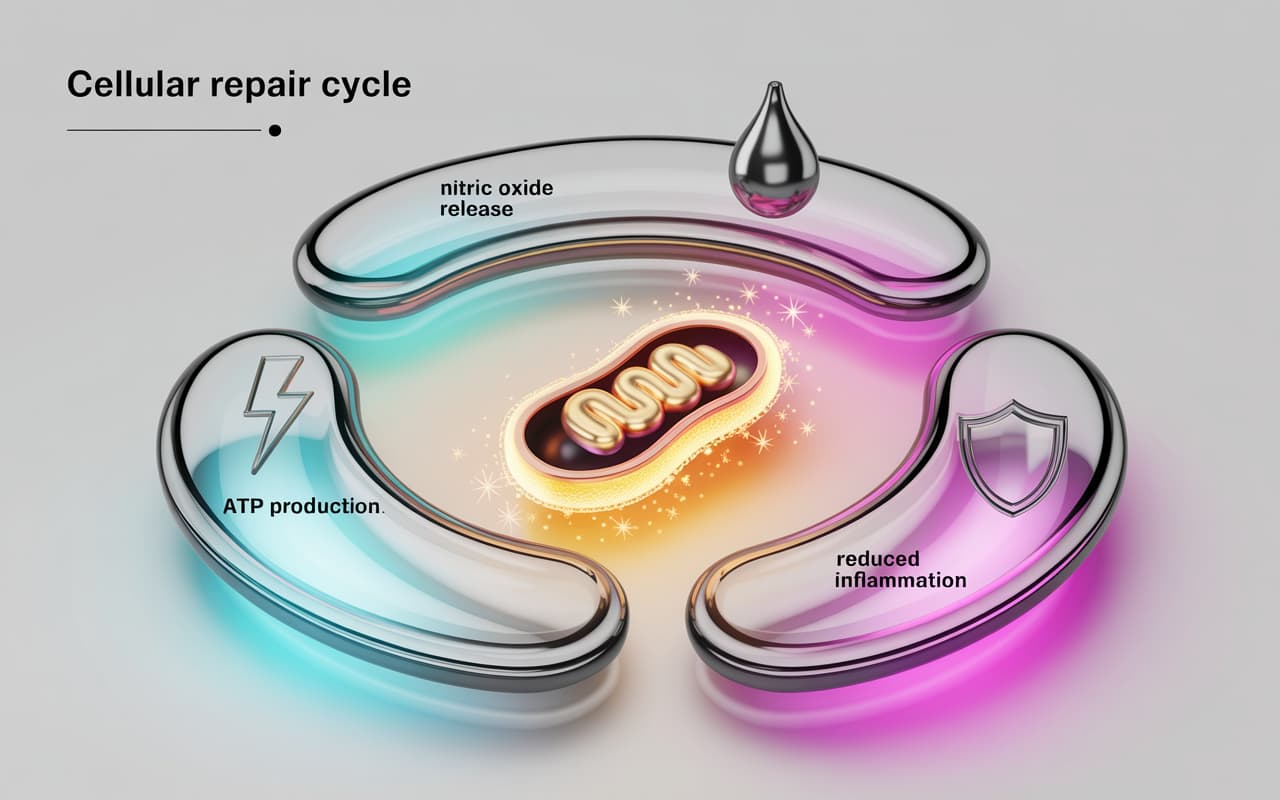
The therapeutic effects of laser therapy are rooted in well-documented biochemical processes. When specific wavelengths of light penetrate tissue, they interact with a enzyme called cytochrome c oxidase located in the mitochondria—the energy-producing organelles within cells.
The Cellular Energy Crisis After Injury
When soft tissue experiences trauma—whether from a car accident, repetitive stress, or degenerative disease—the affected cells enter a state of “metabolic crisis.” Inflammation restricts oxygen delivery, and damaged mitochondria struggle to produce adequate adenosine triphosphate (ATP), the molecular currency of cellular energy. Without sufficient ATP, cells cannot effectively repair damaged proteins, clear inflammatory byproducts, or rebuild structural components like collagen fibers.
The Photobiomodulation Response
Photobiomodulation addresses this crisis through three primary mechanisms:
ATP Production Enhancement: Light in the 600-1000nm range is absorbed by cytochrome c oxidase, increasing the efficiency of the electron transport chain. Studies published in the Journal of Photochemistry and Photobiology have demonstrated ATP increases of 150-200% in treated tissues within minutes of laser application.
Nitric Oxide Displacement: Injured tissues accumulate nitric oxide, which binds to cytochrome c oxidase and blocks ATP synthesis. Photobiomodulation causes nitric oxide to dissociate from the enzyme, simultaneously restoring energy production and causing the released nitric oxide to trigger vasodilation—bringing fresh oxygen and nutrients to the injury site.
Reactive Oxygen Species (ROS) Modulation: Low-level light exposure creates a brief, controlled increase in reactive oxygen species. This hormetic response activates cellular repair pathways, including upregulation of heat shock proteins and growth factors that support tissue regeneration.
The cumulative effect is a tissue environment optimized for repair: increased energy availability, enhanced blood flow, reduced inflammation, and activated healing cascades.
Class IV vs. Class III Lasers: Penetration Depth & Clinical Outcomes
Not all therapeutic lasers deliver equivalent results. The distinction between Class III (“cold laser”) and Class IV (“high-intensity laser”) devices is clinically significant.
Technical Specifications
Class III Lasers operate at power outputs below 500 milliwatts. They produce minimal thermal effect and are limited to treating superficial tissues—typically penetrating 0.5 to 2 centimeters below the skin surface. Treatment sessions often require 20-30 minutes of application time.
Class IV Lasers operate between 500 milliwatts and 60 watts, with most clinical devices in the 10-15 watt range. This higher power density creates a comfortable warming sensation and achieves therapeutic photon density at depths of 5-10 centimeters—reaching deep spinal muscles, intervertebral discs, and nerve roots.
Clinical Implications
The power difference translates directly to treatment efficacy for musculoskeletal conditions. A 2018 systematic review published in Lasers in Medical Science analyzed 47 controlled trials comparing Class III and Class IV lasers for chronic neck and back pain. Class IV treatments demonstrated:
- 40% greater pain reduction scores at 12-week follow-up
- Treatment times reduced to 5-8 minutes (versus 20-30 minutes for Class III)
- Superior outcomes for deep tissue conditions (disc pathology, spinal stenosis, deep ligament injuries)
For Colorado patients dealing with motor vehicle accident injuries—where whiplash often involves deep cervical ligament damage and disc trauma—the penetration depth of Class IV lasers offers access to tissues that manual therapy and Class III devices cannot effectively reach.
The Warming Sensation: Photothermal Effects
Class IV lasers produce a gentle warming effect during treatment. This is therapeutically beneficial. The mild temperature increase (typically 1-2 degrees Celsius in target tissues) enhances metabolic activity and creates a soothing sensation that many patients find immediately relaxing. This is distinct from ablative lasers used in surgery—therapeutic Class IV lasers never cause burns or tissue damage when properly calibrated.
Clinical Applications: When Laser Therapy Is Most Effective
Photobiomodulation has earned FDA 510(k) clearance for specific clinical indications based on peer-reviewed research demonstrating efficacy.
Acute Soft Tissue Trauma
Whiplash and Cervical Acceleration-Deceleration Injuries: The forces involved in rear-end collisions cause microscopic tearing of cervical ligaments and muscle fibers. These injuries are often invisible on standard X-rays but cause profound pain and dysfunction. Laser therapy applied within the first two weeks post-injury has been shown to reduce inflammatory markers (such as prostaglandin E2 and interleukin-6) and accelerate collagen synthesis. Clinical protocols typically involve daily or every-other-day treatment for the first two weeks, transitioning to twice-weekly sessions as acute inflammation resolves.
Contusions and Deep Tissue Bruising: Blunt trauma creates hematomas—pools of blood and inflammatory fluid that impair healing. Photobiomodulation increases lymphatic drainage and macrophage activity, accelerating the clearance of cellular debris and reducing the characteristic purple discoloration and swelling.
Chronic Pain Conditions
Degenerative Disc Disease: While laser therapy cannot reverse disc degeneration, it effectively manages the inflammatory component that drives pain. By reducing the production of inflammatory cytokines in the annular fibers surrounding damaged discs, patients often experience significant pain relief and improved function. Treatment combined with spinal decompression therapy provides synergistic benefits.
Tendinitis and Ligament Inflammation: Chronic overuse injuries to tendons (Achilles, rotator cuff, patellar tendon) and ligament strains respond well to laser therapy. The increased ATP production supports the energy-intensive process of collagen remodeling—the mechanism by which damaged connective tissue is gradually replaced with healthy, organized fibers.
Osteoarthritis: Joint degeneration creates chronic low-grade inflammation in synovial membranes. Studies in osteoarthritis of the knee have shown that laser therapy can reduce joint effusion (swelling) and improve range of motion, though effects are typically temporary and require ongoing maintenance treatments.
Neuropathic Conditions
Radiculopathy (Sciatica): When herniated discs or bone spurs compress nerve roots, the resulting inflammation causes radiating pain, numbness, and weakness. Laser therapy applied along the path of the affected nerve can reduce inflammatory mediators and support nerve membrane repair. Many patients report decreased burning and tingling sensations within 3-5 treatment sessions.
Peripheral Neuropathy: Damage to small nerve fibers in the extremities—whether from diabetes, chemotherapy, or trauma—often causes burning foot pain and balance problems. Emerging research suggests that photobiomodulation may support nerve regeneration through upregulation of nerve growth factor (NGF) and brain-derived neurotrophic factor (BDNF), though this application requires longer treatment courses (12-20 sessions).
Post-Surgical Rehabilitation
Laser therapy is increasingly used to manage post-operative pain and accelerate wound healing. The treatment is safe to apply over surgical incisions (once sutured) and internal hardware such as titanium plates or screws. By reducing scar tissue formation and improving tissue oxygenation, photobiomodulation can shorten recovery timelines following spinal surgery, joint replacements, or soft tissue repair procedures.
The Treatment Experience: Protocols, Frequency & Timeline
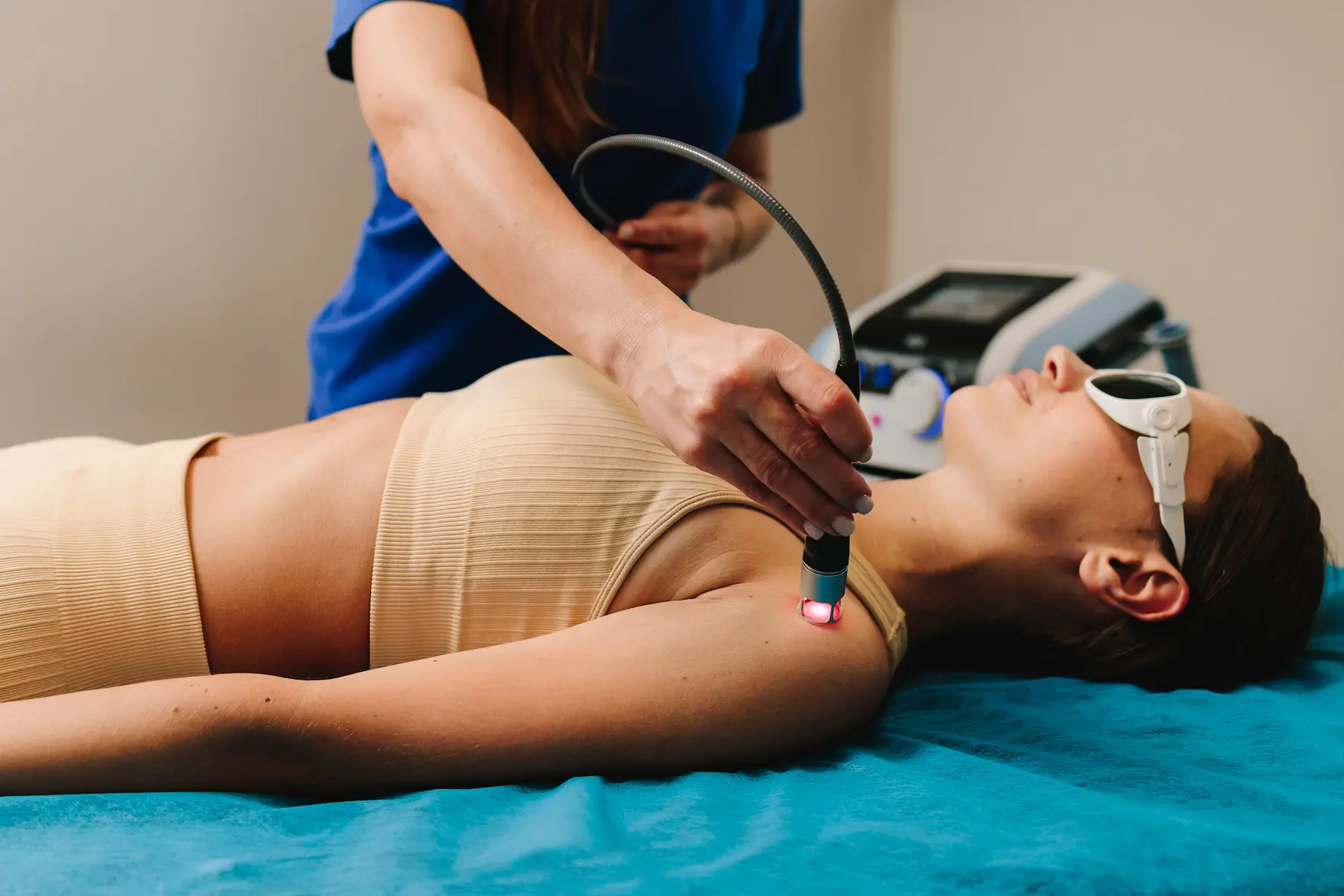
Understanding what to expect during laser therapy helps patients engage actively in their recovery process.
During a Typical Session
Treatment begins with the patient positioned comfortably—either lying prone, supine, or seated depending on the treatment area. The clinician uses a handheld applicator that delivers laser energy through a focused beam or diffused lens. The applicator is moved slowly across the treatment zone in a grid pattern or held stationary over specific points.
Most patients report a gentle, soothing warmth penetrating deep into the tissue. There is no pain, no electrical sensation, and no need for topical anesthetics. Sessions typically last 5-12 minutes depending on the size of the treatment area and the power density of the device.
Patients remain fully clothed, though metal jewelry should be removed from the treatment area. The clinician and patient wear protective eyewear specific to the laser wavelength being used.
Treatment Frequency
Acute Conditions (less than 6 weeks old): Aggressive initial treatment yields best results. Protocols often call for daily sessions for the first week, then 3 times weekly for weeks 2-4, then tapering to weekly as symptoms resolve. Total treatment course: 10-15 sessions.
Chronic Conditions (more than 3 months duration): Tissues in chronic pain states have adapted to dysfunction and require consistent stimulation to shift toward healing. Typical protocols involve twice-weekly treatments for 6-8 weeks (12-16 sessions), followed by monthly maintenance treatments as needed.
Post-Surgical Recovery: Treatment can often begin 3-5 days post-surgery (once acute surgical inflammation peaks). Three times weekly for 3-4 weeks supports optimal wound healing.
Expected Timeline for Results
Response to laser therapy follows a general pattern, though individual variation is significant:
- Sessions 1-3: Many patients report immediate relaxation and slight pain reduction lasting several hours post-treatment. This early response is primarily due to pain gating mechanisms (temporary desensitization of nociceptors) rather than tissue healing.
- Sessions 4-8: Cumulative cellular effects become apparent. Pain reduction becomes more sustained, morning stiffness decreases, and range of motion begins to improve. This reflects actual tissue repair—collagen remodeling, reduced inflammatory markers, and improved local circulation.
- Sessions 9+: Functional improvements plateau. At this stage, treatment frequency is often reduced, and the focus shifts to maintaining gains and preventing regression.
It is important to note that laser therapy does not produce instant, permanent “cures.” Like physical therapy or nutritional interventions, it supports the body’s own repair processes, which unfold according to biological timelines.
Safety Profile: Contraindications, Side Effects & Device Clearance
Class IV laser therapy has an established safety record when administered by trained clinicians following evidence-based protocols.
FDA Clearance Status
Therapeutic lasers are classified as Class II medical devices under FDA regulations. Manufacturers must demonstrate safety and efficacy through 510(k) premarket notification, showing that their devices are substantially equivalent to previously cleared devices. Class IV lasers have received clearance for indications including temporary relief of minor muscle and joint pain, arthritis pain, muscle spasm, and stiffness, as well as increasing local blood circulation.
The FDA clearance process requires manufacturers to document wavelength specifications, power output calibration, safety features (such as emergency shutoffs), and clinical trial data supporting therapeutic claims.
Contraindications (When Not to Use Laser Therapy)
Certain conditions require caution or absolute avoidance:
Pregnancy: Laser therapy should not be applied over the abdomen or lower back of pregnant patients. While there is no evidence of harm, the precautionary principle applies due to limited research in this population.
Active Cancer or Suspicious Lesions: Photobiomodulation should not be applied directly over known malignancies or undiagnosed masses, as the treatment stimulates cellular activity and could theoretically accelerate tumor growth.
Photosensitizing Medications: Patients taking certain medications (some antibiotics, retinoids, or chemotherapy agents) may have increased light sensitivity. Clinicians should review medication lists before treatment.
Directly Over the Eyes: Though Class IV lasers are safe for skin and deep tissues, direct exposure to the retina can cause damage. Both clinician and patient wear wavelength-specific protective eyewear throughout treatment.
Safety with Medical Devices
Metal Implants: Class IV laser therapy is completely safe to use over titanium plates, screws, joint replacements, and other metallic hardware. The laser energy does not heat metal significantly and poses no risk of burns or device malfunction.
Pacemakers: Current research suggests that laser therapy does not interfere with pacemaker function, as it does not produce electromagnetic fields. However, conservative protocols avoid directing the laser beam directly over the pacemaker unit itself.
Side Effects
Adverse effects from properly administered Class IV laser therapy are rare and typically mild:
- Temporary Increase in Pain: Approximately 5-10% of patients report a brief increase in pain following their first 1-2 treatments. This is thought to reflect increased metabolic activity in chronically dysfunctional tissues and typically resolves within 24-48 hours.
- Fatigue: Some patients feel unusually tired following treatment, likely due to the energy demands of accelerated tissue repair.
- Skin Sensitivity: Rarely, patients may experience mild redness or warmth at the treatment site lasting several hours.
There are no reported cases of burns, tissue damage, or permanent complications when Class IV lasers are used according to manufacturer guidelines by trained providers.
The Medico-Legal Documentation Advantage: Colorado Auto Injury Claims
For Colorado patients pursuing personal injury claims following motor vehicle accidents, the documentation generated during laser therapy serves an important secondary function: objective evidence of injury severity and treatment necessity.
The “Soft Tissue Injury” Problem
Insurance adjusters frequently attempt to minimize the value of whiplash and soft tissue injury claims, arguing that pain complaints are subjective and that diagnostic imaging (X-rays, MRI) shows “minimal findings.” This creates a documentation gap that disadvantages injured patients.
AMA Guidelines and Objective Treatment Records
The American Medical Association’s Guides to the Evaluation of Permanent Impairment recognizes that soft tissue injuries can cause long-term functional limitations even when structural damage is not visible on imaging. Treatment records that document specific therapeutic interventions—including photobiomodulation protocols—establish the medical necessity and severity of the injury.
Each laser therapy session generates clinical documentation including:
- Treatment parameters (wavelength, power density, duration)
- Anatomical areas treated
- Patient-reported pain levels (visual analog scale)
- Functional assessments (range of motion, orthopedic tests)
This creates a longitudinal record demonstrating both the extent of treatment required and the patient’s progress (or lack thereof), which becomes critical evidence in settlement negotiations or litigation.
Colorado Med-Pay Coverage
Most Colorado auto insurance policies include Medical Payments coverage (Med-Pay)—a no-fault benefit that covers reasonable and necessary medical treatment arising from motor vehicle accidents, typically up to $5,000-$50,000 depending on policy limits.
Photobiomodulation therapy is generally covered under Med-Pay when properly documented using appropriate CPT codes (97039 for unlisted modality, or 97026 for infrared therapy, depending on carrier guidelines). Clinics experienced in auto accident injury management handle the billing and documentation required to ensure coverage.
Lien-Based Treatment
For patients whose Med-Pay has been exhausted or who do not have health insurance, many Colorado chiropractic clinics offer treatment on a medical lien basis—meaning treatment is provided with payment deferred until the personal injury case settles. This ensures that financial constraints do not delay necessary care.
Frequently Asked Questions About Laser Therapy
How does laser therapy differ from ultrasound or shockwave therapy?
While all three modalities use energy to stimulate tissue repair, they work through different mechanisms. Ultrasound uses high-frequency sound waves to create mechanical vibration and heat in tissues, which increases circulation and breaks up scar tissue. Shockwave therapy delivers high-energy acoustic pulses that create controlled microtrauma to stimulate healing responses. Laser therapy, by contrast, uses light energy absorbed directly by cellular structures (specifically mitochondria) to increase ATP production and modulate inflammation at a biochemical level. These treatments are often complementary rather than competitive—many protocols combine laser therapy with other modalities for synergistic effects.
Is high-intensity laser therapy painful during the treatment?
No. Class IV laser therapy produces a gentle, soothing warmth that most patients find relaxing. There is no electrical sensation, no needles, and no discomfort. The warming effect is therapeutically beneficial and distinctly different from the heat produced by heating pads or hot packs—it represents energy being absorbed deep within tissues rather than superficial skin warming. Some patients even fall asleep during treatment sessions.
How many sessions are typically required to treat chronic back pain?
Treatment response depends on the duration and severity of the condition. For chronic low back pain that has persisted for months or years, research protocols typically involve 12-16 sessions delivered over 6-8 weeks (twice weekly). Many patients report noticeable improvement by sessions 5-7, with continued gains as treatment progresses. Chronic conditions often require periodic maintenance treatments (monthly or quarterly) to sustain benefits, as laser therapy does not “cure” degenerative processes but rather manages inflammation and supports ongoing tissue health.
Can laser therapy be safely used over titanium implants or pacemakers?
Yes, Class IV laser therapy is safe to use over metal implants including titanium plates, screws, joint replacements, and dental implants. The laser energy does not significantly heat metal or cause any device malfunction. For patients with pacemakers, current research indicates no interference with device function, though conservative practice avoids directing the laser beam directly over the pacemaker generator unit itself. Always inform your provider of any implanted medical devices before treatment.
What are the potential side effects of Class IV laser therapy?
Side effects are rare and typically mild. Approximately 5-10% of patients experience a temporary increase in pain following their first 1-2 treatments, which usually resolves within 24-48 hours. Some patients report feeling tired after treatment, likely due to increased metabolic activity. Skin redness or warmth at the treatment site may occur but is uncommon and short-lived. There are no reported cases of burns, tissue damage, or serious complications when treatment is administered by trained providers following manufacturer protocols.
Is laser therapy covered by standard medical insurance or Medicare?
Coverage varies by insurance carrier and policy type. For Colorado auto accident injuries, laser therapy is typically covered under Medical Payments (Med-Pay) provisions. Medicare covers laser therapy for specific conditions when criteria are met, though coverage can be limited. Private insurance coverage is inconsistent—some carriers cover photobiomodulation for pain management while others consider it investigational. Many chiropractic clinics offer complimentary insurance verification before beginning treatment, and some offer cash-pay rates or payment plans for patients whose insurance does not provide coverage.
How long does the pain relief last after a single session?
Initial sessions often provide 2-6 hours of pain relief, primarily due to temporary effects on pain receptors. As treatments accumulate, pain relief becomes more sustained, reflecting actual tissue healing rather than symptom masking. By sessions 6-10, many patients experience pain reduction lasting days rather than hours. For chronic conditions, periodic maintenance treatments (every 2-4 weeks) often sustain benefits long-term. It is important to understand that laser therapy is not an instant permanent “fix” but rather a tool that supports the body’s repair processes over time.
Does laser therapy work for nerve damage and numbness?
Emerging research suggests photobiomodulation may support nerve regeneration and reduce neuropathic pain. For conditions like sciatica (where nerve roots are inflamed but not permanently damaged), laser therapy can reduce inflammation and improve symptoms relatively quickly. For true nerve damage—such as peripheral neuropathy from diabetes or chemotherapy—the effects are more variable. Some patients experience meaningful improvements in burning pain and sensation, while others see minimal benefit. Nerve regeneration is a slow process measured in months, so realistic expectations and longer treatment courses (15-20 sessions) are typically required for neuropathic conditions.
Can I combine laser therapy with other treatments like chiropractic adjustments?
Yes, combination therapy is often ideal. Laser therapy prepares tissues by reducing inflammation and muscle guarding, which allows for more comfortable and effective manual adjustments. Many clinicians apply laser therapy immediately before spinal manipulation or soft tissue work. The treatments are synergistic—manual therapy restores proper joint mechanics while laser therapy supports the cellular repair needed for long-term healing. Discussing an integrated treatment plan with your provider ensures all modalities work together efficiently.
Is there any research supporting laser therapy, or is it experimental?
Laser therapy is supported by substantial peer-reviewed research. The National Institutes of Health’s PubMed database contains over 4,000 published studies on photobiomodulation for pain management, wound healing, and tissue repair. A 2018 Cochrane Review (considered the gold standard for medical evidence synthesis) concluded that low-level laser therapy provides short-term pain relief and functional improvement for chronic neck pain. While research quality varies, the fundamental mechanisms of photobiomodulation—ATP enhancement, nitric oxide modulation, and anti-inflammatory effects—are well-established in cellular biology. The therapy is not experimental; it is an evidence-based intervention with FDA clearance for specific clinical applications.