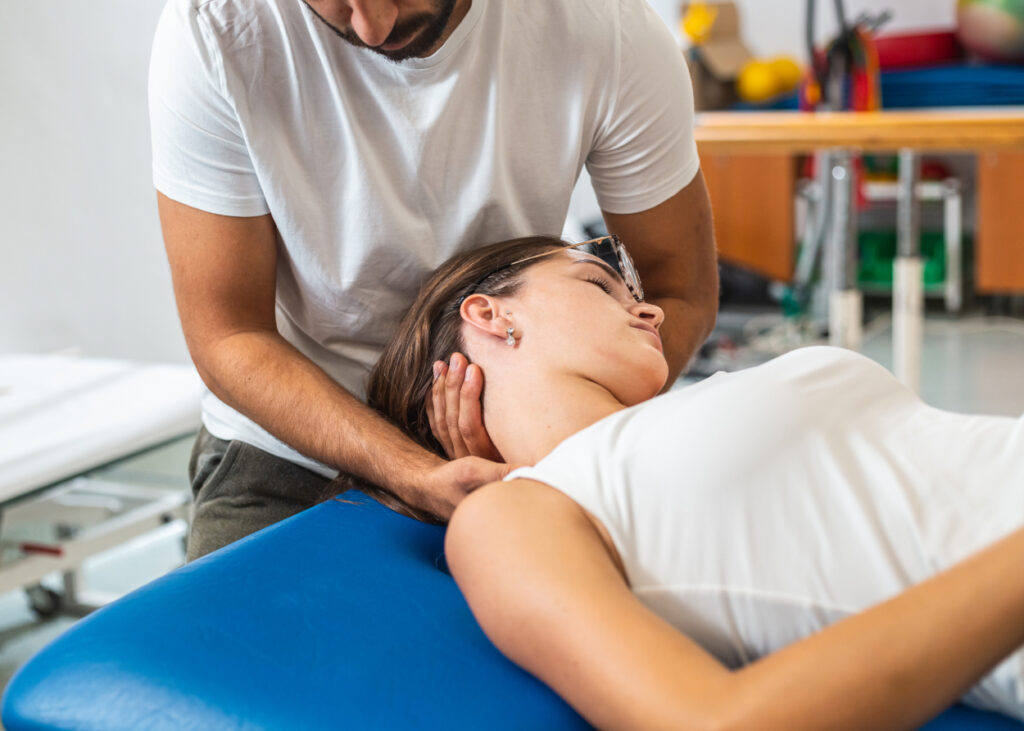
Key Takeaways
- A vehicle can absorb almost all visible impact in a low-speed collision while the occupant’s cervical spine absorbs a disproportionate amount of force — this is the core biomechanical reason “minor damage” does not equal “minor injury.”
- Muscle guarding — a neurochemical reflex — can chemically suppress pain at the scene, causing symptoms to peak 48–72 hours after impact. Feeling fine initially is clinically expected, not a sign you are uninjured.
- Standard X-rays often cannot detect soft tissue and ligament injuries. Advanced diagnostics, such as Digital Motion X-ray (DMX), may reveal instability that conventional imaging misses.
- Colorado Med-Pay coverage may help cover eligible medical expenses regardless of fault. Comprehensive documentation adhering to AMA guidelines can be critical to protecting both your health recovery and your insurance claim.
In a low-speed rear-end collision, a vehicle’s bumper and crumple zones are engineered to absorb and dissipate impact energy, which is exactly why the car may look fine. The problem is that the energy that doesn’t deform the vehicle has to go somewhere. Research suggests a significant portion of that force transfers directly through the seat and into the occupant’s cervical spine in a fraction of a second, often before the occupant can brace.
This is the foundational reason why neck and back pain after a minor accident is not imagined, exaggerated, or unusual. It is a predictable biomechanical outcome — and understanding it is the first step toward protecting your health and your claim.
Why Does a Minor Fender-Bender Cause Major Pain?
The common assumption — “if the car isn’t damaged, I can’t be injured” — is one of the most persistent myths in post-accident care. It is also one that insurance adjusters sometimes rely on to minimize claims.
Here is what the physics actually show. Modern vehicle bumpers are specifically designed to absorb low-speed impacts (typically under 10 mph) with minimal structural damage. That engineering success means the kinetic energy of the collision is not dissipated through crumpling metal. Instead, it is transferred through the rigid frame of the vehicle, through the seat, and into the occupant’s body.
Studies in crash biomechanics have found that even collisions at speeds as low as 5–8 mph can generate forces sufficient to strain cervical soft tissues. The vehicle sustains little or no visible damage precisely because it performed as designed. The human spine, by contrast, is not engineered to absorb that kind of sudden, unbraced loading — particularly in a rear-impact scenario where the head and neck lag behind the torso during acceleration.
The disconnect between vehicle damage and occupant injury is not a legal argument. It is an established principle in biomechanics research.
What Is Cervical Acceleration-Deceleration — and Why Does It Matter?
Cervical Acceleration-Deceleration (CAD) — commonly referred to as whiplash — describes the specific motion pattern the head and neck undergo during a rear-impact collision. Understanding the sequence helps explain why the injuries are so often delayed and so frequently misunderstood.
In a typical rear-end impact, the sequence unfolds in roughly 300 milliseconds:
- The torso accelerates forward as the seat pushes it, driven by the vehicle’s sudden change in velocity.
- The head lags behind due to inertia, causing the lower cervical spine to hyperextend (bend backward) while the upper cervical spine simultaneously flexes (bends forward).
- The head then snaps forward as the ligaments and muscles reach their stretch limit, creating a secondary hyperflexion phase.
This “S-curve” deformation of the cervical spine happens faster than the human neuromuscular system can respond. The muscles simply do not have time to contract and protect the joints before the injury-producing forces are already acting on the soft tissues, ligaments, and intervertebral discs.
This is why Cervical Acceleration-Deceleration is classified as a distinct injury mechanism — not just “a sore neck” — and why trauma-informed care that addresses the full biomechanical picture may support a more complete recovery than general wellness adjustments alone.
Why Didn’t I Feel It at the Scene? The Science of Muscle Guarding
One of the most clinically important — and least discussed — aspects of low-speed collision injuries is why so many people feel relatively fine immediately after the crash, only to wake up 48 to 72 hours later in significant pain.
The answer lies in a neurochemical reflex called muscle guarding.
At the moment of impact, the body’s sympathetic nervous system activates a protective cascade. Adrenaline (epinephrine) and other stress hormones flood the system, acutely elevating pain thresholds and temporarily masking the sensation of soft tissue strain. Simultaneously, the muscles surrounding the injured area contract reflexively and forcefully — “guarding” the damaged structures. This splinting effect can make the neck feel stiff but functional, rather than acutely painful.
Over the following 24 to 72 hours, several processes converge to reveal the true extent of the injury:
- Cytokine release — the body’s inflammatory signaling molecules — ramps up as the immune response to microtrauma in the ligaments and muscle fibers accelerates.
- Neuro-inflammation develops around irritated nerve roots, contributing to radiating pain, headaches, and cognitive symptoms sometimes described as “brain fog.”
- Muscle guarding fatigue sets in, and the protective splinting that was masking pain begins to break down.
This is why the 48–72 hour window is clinically significant. Feeling fine at the accident scene is not evidence of no injury. It is, in many cases, a predictable physiological response to acute trauma. Documenting symptoms as they evolve — beginning as soon as possible after the collision — is important both for your recovery and for any insurance or legal process that may follow.
What Symptoms Should I Watch For in the First 72 Hours?
Symptoms following a low-speed collision can appear gradually and may involve more than just the neck. Some people experience one or two of the following; others experience several. This list is for general informational purposes and is not a substitute for a clinical evaluation.
Musculoskeletal symptoms:
- Neck stiffness or reduced range of motion
- Upper back or shoulder pain
- Tenderness along the base of the skull or between the shoulder blades
- Jaw pain or difficulty opening the mouth fully (TMJ involvement)
Neurological symptoms:
- Headaches, particularly at the base of the skull
- Tingling, numbness, or a “pins and needles” sensation in the arms or hands
- Dizziness or a sense of imbalance
Cognitive and systemic symptoms:
- Difficulty concentrating or memory gaps (“brain fog”)
- Unusual fatigue or sleep disruption
- Increased sensitivity to light or sound
Seek urgent or emergency care immediately if you experience severe or rapidly worsening pain, loss of consciousness, significant weakness in the arms or legs, difficulty swallowing or breathing, or any symptom that concerns you. These may indicate a more serious injury requiring immediate evaluation.
For symptoms that are present but not acutely severe, a licensed clinician with experience in auto-injury traumatology can perform a structured evaluation — including range-of-motion testing and neurological screening — to document your presentation objectively.
Why Standard X-Rays Often Miss These Injuries
It is common for accident victims to be told their X-rays or MRI came back “normal” — and yet remain in significant pain. This is not a contradiction. It is a reflection of what standard imaging is and is not designed to detect.
Conventional X-rays capture bone structure in a static, fixed position. They are effective at identifying fractures and gross skeletal misalignment. They are not designed to detect ligament laxity — the stretching or partial tearing of the stabilizing ligaments of the cervical spine — which is one of the most common and clinically significant injuries in Cervical Acceleration-Deceleration trauma.
Digital Motion X-ray (DMX) is an advanced diagnostic tool that captures real-time, dynamic imaging of the spine in motion. By evaluating the cervical vertebrae as they move through their full range, DMX can reveal abnormal segmental motion and ligament instability that a static X-ray simply cannot show.
This distinction matters enormously for two reasons. First, undetected ligament laxity that goes untreated may contribute to chronic instability and long-term pain. Second, from a documentation standpoint, a “normal” static X-ray in the context of a personal injury claim does not mean the injury does not exist — it means the right diagnostic tool may not have been used yet.
Providers who specialize in auto-injury traumatology and adhere to AMA documentation guidelines understand this distinction and can order appropriate advanced diagnostics when clinically indicated.
How Does Documentation Protect Your Recovery — and Your Claim?
The medical record created in the days and weeks after a collision serves two parallel purposes: it guides your clinical care, and it creates the evidentiary record that supports your insurance claim or legal case.
Comprehensive documentation — adhering to AMA guidelines — typically includes objective findings such as:
- Range-of-motion measurements using a clinical inclinometer (not estimated)
- Neurological screening (reflex testing, dermatomal sensory mapping)
- Orthopedic provocation tests specific to cervical and lumbar injury patterns
- Diagnostic imaging reports, including any advanced imaging such as DMX
- A documented symptom timeline that captures onset, progression, and functional limitations
This level of documentation matters because insurance adjusters evaluating a soft tissue injury claim are looking for objective clinical evidence, not subjective pain reports alone. A claim supported by thorough, AMA-compliant records from a verified specialist is substantively different from one supported only by a single urgent care visit.
Colorado Med-Pay (Medical Payments coverage) may help cover eligible medical expenses — including chiropractic and specialist care — regardless of who was at fault in the collision. Coverage varies by policy, so confirming your specific benefits with your insurer is an important early step. A provider experienced in Colorado auto-injury claims can help ensure that treatment is billed and documented in a manner consistent with your coverage.
Understanding your options and documentation needs early in the process — rather than weeks later — can make a meaningful difference in both your clinical outcome and your claim.
Frequently Asked Questions
Can a 5 mph car crash cause whiplash?
Research suggests that cervical soft tissue injuries can occur at impact speeds as low as 5–8 mph. The determining factor is not vehicle speed alone, but the rate of change in velocity (delta-V), the occupant’s position at the moment of impact, and whether the muscles had time to brace. A licensed clinician can evaluate whether your specific symptoms are consistent with a low-speed collision mechanism.
Why does my neck hurt if my car has no damage?
Modern vehicle bumpers are engineered to absorb low-speed impacts without visible structural damage. That engineering success means the collision energy transfers into the occupant rather than deforming the vehicle. Neck pain after a collision with no visible car damage is a recognized and biomechanically predictable outcome — not an indication that the injury is fabricated.
What is the delayed onset of whiplash symptoms?
Delayed onset is primarily driven by the muscle guarding response and subsequent neuro-inflammatory cascade described above. Adrenaline and protective muscle contraction can mask pain at the scene. As those mechanisms subside and cytokine-driven inflammation develops over 24–72 hours, symptoms typically become more apparent. Documenting symptoms as they evolve is clinically and legally important.
How do you prove a soft tissue injury from a minor car accident?
Objective clinical documentation is the foundation. This includes measured range-of-motion deficits, neurological screening findings, orthopedic test results, and advanced imaging such as DMX when ligament instability is suspected. Documentation standards can matter significantly in claims — talk to your provider and attorney about what is needed for your specific situation.
Will insurance pay for medical bills if there is no car damage?
Colorado Med-Pay coverage may help cover eligible medical expenses regardless of the extent of vehicle damage or fault determination. Coverage varies by policy; confirming your specific benefits with your insurer is an important first step. A provider with experience in Colorado auto-injury claims can help navigate billing and documentation in a way that aligns with your coverage.
What To Do Next
If you were in a collision — even one that seemed minor — and you are now experiencing neck pain, stiffness, headaches, or any of the symptoms described above, the most important thing you can do is get evaluated promptly.
Waiting to see if symptoms resolve on their own is understandable. But the window for establishing a documented clinical baseline is narrow, and gaps in the medical record can create complications for both your recovery and your claim.
Connect with verified specialists in Colorado’s auto-injury chiropractic and physical medicine network who understand Cervical Acceleration-Deceleration, AMA documentation standards, and Colorado Med-Pay laws.
Don’t navigate your recovery alone. Trauma-informed care — grounded in biomechanics and built around your specific documentation needs — may make a meaningful difference in what comes next.
 Colorado Med‑Pay Laws: 3 Practical and Policy-Safe Ways To Work With the System
Colorado Med‑Pay Laws: 3 Practical and Policy-Safe Ways To Work With the System