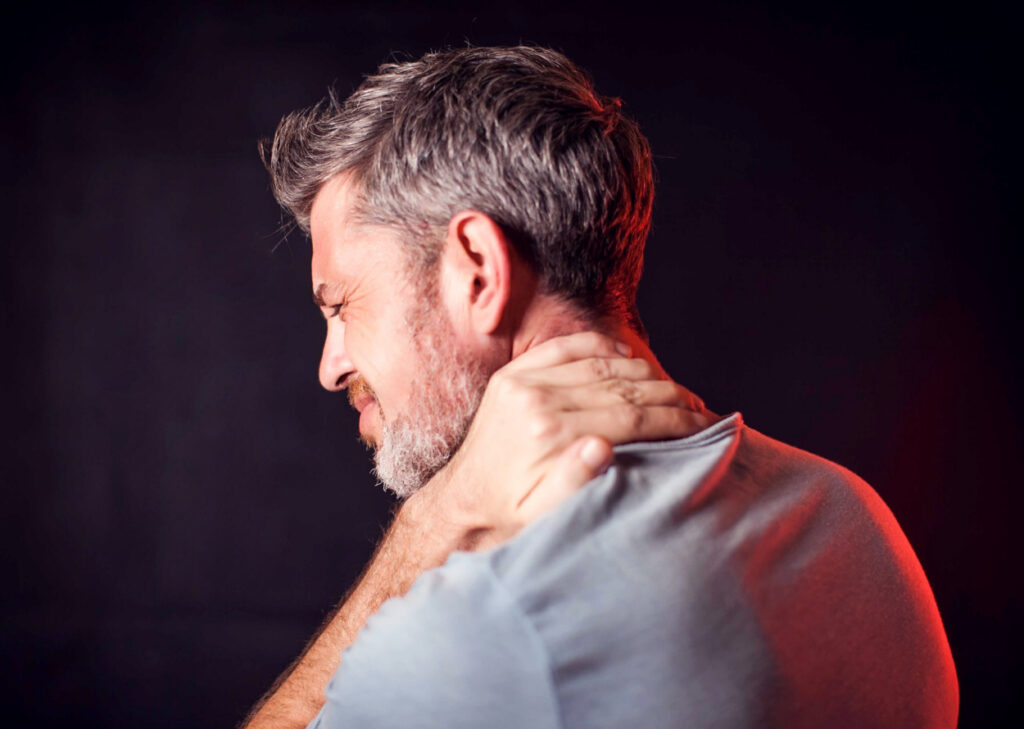
Key Takeaways
- Whiplash pain commonly intensifies 24–72 hours after a collision due to adrenaline masking early symptoms and a delayed inflammatory cascade involving cytokine release — not because the injury is “minor.”
- Cervical Acceleration-Deceleration (CAD) can cause micro-tears in soft tissue, ligament laxity, and neuro-inflammation that standard emergency room X-rays are not designed to detect.
- Colorado Med-Pay coverage may help cover the cost of delayed whiplash treatment, depending on your policy, even if you didn’t seek care at the scene.
- Connecting with a specialist trained in auto accident biomechanics — and getting properly documented — can be critical to both your recovery and any future insurance claim.
If you walked away from a car collision feeling relatively okay — and now, two or three days later, you can barely turn your head — you are not imagining it. You are not being dramatic. What you are experiencing is a predictable, well-documented physiological response to cervical trauma, and it has a name: Cervical Acceleration-Deceleration (CAD) syndrome.
The delayed onset of whiplash symptoms is one of the most misunderstood phenomena in auto accident medicine. This guide explains, in plain terms, exactly what is happening inside your cervical spine — and why getting a proper evaluation now, rather than waiting, may matter more than you realize.
Why Does Whiplash Pain Appear Days After the Crash?
The short answer: your body’s emergency systems worked against you.
At the moment of impact, your nervous system floods your bloodstream with adrenaline (epinephrine) and cortisol — the same hormones that allow people to lift cars off of trapped children. These stress hormones are powerful, fast-acting analgesics. They suppress pain signals so effectively that many collision victims genuinely feel fine at the scene, pass a basic ER assessment, and go home believing the worst is over.
It isn’t. The adrenaline clears your system within hours. What it leaves behind is injured tissue.
As the hormonal mask fades, your immune system begins its damage-assessment process. Specialized proteins called cytokines are released into the affected area — the muscles, ligaments, and nerves of your cervical spine. Cytokines are pro-inflammatory signals; their job is to recruit healing cells to the injury site. But that inflammatory cascade also produces swelling, pressure on nerve roots, and the deep, spreading ache that many patients describe as “waking up feeling like I was hit by a truck.”
Research published in peer-reviewed journals on soft tissue biomechanics consistently identifies this neuro-inflammatory delay as the primary mechanism behind worsening post-crash pain. The injury happened at impact. The pain arrives with a delay.
What Actually Happens to Your Cervical Spine During a Collision
Picture your cervical spine —the seven vertebrae of your neck— as a precisely stacked column of bones, each cushioned by a disc and stabilized by an intricate web of ligaments and muscles. Under normal conditions, this system absorbs the stresses of daily movement gracefully.
During a rear-end or side-impact collision, that system is subjected to forces it was never designed to handle.
In the fraction of a second after impact, your torso is driven forward by the seat while your head — weighing approximately 10–12 pounds — lags behind due to inertia. Your cervical spine undergoes a rapid, S-shaped deformation: the lower vertebrae are forced into hyperextension while the upper vertebrae simultaneously flex forward. This motion happens faster than your muscles can reflexively contract to protect you — typically in 150–300 milliseconds, well below the human reflex threshold of approximately 800 milliseconds.
The result is a biomechanical event that can cause:
- Micro-tears in the paraspinal muscles and cervical ligaments
- Anterior and posterior longitudinal ligament strain, compromising spinal stability
- Facet joint capsule injury, a common but frequently overlooked source of chronic neck pain
- Intervertebral disc disruption, including annular tears that may not be visible on standard imaging
- Nerve root irritation, which can produce radiating pain, numbness, or tingling into the arms and hands
This is why a collision that appears minor by vehicle damage standards can produce significant cervical injury. The energy transferred to the occupant’s spine does not always correlate with the severity of the vehicle impact.
The Delayed Trauma Timeline — What Your Body Is Doing in the First 72 Hours
Understanding where you are in the biological response to your injury can help reduce the anxiety of “why am I getting worse?” Here is a general timeline of what the research suggests typically occurs. Individual experiences vary, and this is not a substitute for a clinical evaluation.
0–6 Hours Post-Impact: The Adrenaline Window
Most people feel minimal pain or localized stiffness at most. The sympathetic nervous system is still activated. Many collision victims drive themselves home, go to work, or decline emergency transport at the scene. This is common — and it does not mean the injury is absent.
6–24 Hours: The Inflammatory Onset
As stress hormones clear, the immune system’s inflammatory response begins. Cytokines signal increased blood flow and cellular activity to the injured cervical tissues. Patients typically begin noticing:
- Stiffness and reduced range of motion in the neck
- A dull, spreading ache that may extend into the upper back and shoulders
- The onset of tension headaches originating at the base of the skull (occipital region)
- Early fatigue or a sense of cognitive heaviness
24–72 Hours: Peak Symptom Emergence
This is the window during which most patients describe their symptoms as “worst.” Inflammation peaks, and the full scope of the soft tissue injury becomes symptomatic. Common presentations include:
- Significant neck pain and muscle spasm
- Headaches that may mimic tension or migraine patterns
- Dizziness or balance disturbance (which may indicate vestibular involvement or upper cervical nerve irritation)
- Brain fog, difficulty concentrating, or short-term memory disruption
- Radiating pain, numbness, or tingling into the arms — signs of potential nerve root involvement
This is also the window during which many patients first search for answers online — and the window during which seeking a trauma-informed injury evaluation may be most clinically valuable.
1 Week and Beyond: Chronic Risk and Ligament Laxity
For patients who do not receive appropriate evaluation and care, acute cervical soft tissue injury carries a documented risk of transitioning into chronic pain. Research in the Journal of Orthopaedic & Sports Physical Therapy and related publications suggests that a subset of whiplash patients develop ligament laxity — a permanent reduction in the structural integrity of cervical ligaments — which can cause ongoing instability, recurring headaches, and long-term functional limitations.
Early, accurate diagnosis is associated with better long-term outcomes. Waiting is not without risk.
Why Standard ER X-Rays Often Miss the Injury
One of the most common points of confusion we hear from patients: “The ER said my X-rays were clear — so why do I still feel this bad?”
Standard radiographs (X-rays) are excellent tools for identifying fractures and gross bony abnormalities. They are not designed to image soft tissue. Cervical ligaments, muscle fibers, intervertebral disc annuli, and facet joint capsules are not visible on a standard X-ray. A clear X-ray after a collision means you likely did not fracture a vertebra — it does not mean your soft tissue structures are uninjured.
For patients with persistent or worsening symptoms, more advanced imaging modalities may be appropriate:
- MRI (Magnetic Resonance Imaging): Can visualize disc herniations, annular tears, and significant ligament damage, though it captures a static image of the spine at rest.
- Digital Motion X-Ray (DMX): A specialized fluoroscopic technology that images the cervical spine in motion, allowing clinicians to identify ligament laxity — abnormal vertebral movement patterns that indicate structural instability. DMX is particularly valuable in medical-legal contexts because it provides objective, dynamic evidence of injury that static imaging cannot capture.
The decision to pursue advanced imaging should be made in consultation with a licensed clinician based on your specific presentation. A specialist trained in soft tissue injury rehabilitation can help determine which diagnostic pathway is appropriate for your case.
How Is Ligament Laxity Diagnosed After an Auto Collision?
Ligament laxity refers to the pathological loosening or elongation of cervical ligaments — the connective tissue bands that hold your vertebrae in proper alignment. When these structures are overstretched or micro-torn during a CAD event, the vertebrae they stabilize may begin to move beyond their normal range, creating instability.
Diagnosing ligament laxity typically involves a combination of:
- Clinical examination — assessing range of motion, palpation of cervical structures, and neurological screening
- Stress radiography — specialized X-ray views taken at the extremes of flexion and extension to reveal abnormal vertebral movement
- DMX imaging — the most sensitive tool for capturing dynamic instability in real time
- MRI — to rule out disc herniation or cord involvement
Ligament laxity is clinically significant for two reasons: it can cause ongoing pain and functional limitation, and it is a documented, objective finding that carries weight in insurance claims and personal injury documentation. Specialists trained in auto accident biomechanics understand how to identify, document, and communicate these findings in a format that meets AMA guideline standards.
Red Flag Symptoms That Require Immediate Emergency Care
This section is critical. Do not ignore these signs.
While most delayed whiplash symptoms follow the timeline described above, certain presentations may indicate a more serious injury requiring immediate emergency evaluation. Seek urgent or emergency care if you experience:
- Loss of consciousness or confusion at any point after the collision
- Severe, rapidly worsening headache, unlike any you’ve had before
- Numbness, tingling, or weakness in both arms or both legs simultaneously
- Loss of bladder or bowel control
- Difficulty swallowing or speaking
- Sudden vision changes or double vision
- Fever combined with neck stiffness and sensitivity to light
These symptoms may indicate spinal cord injury, intracranial hemorrhage, or other conditions that require immediate medical intervention. Call 911 or go to the nearest emergency room. Do not drive yourself.
Does Colorado Med-Pay Cover Delayed Whiplash Treatment?
This is one of the most common questions Colorado accident victims have — and the answer is: it depends on your policy, but delayed treatment does not automatically disqualify you.
Colorado requires all auto insurance policies to include Medical Payments (Med-Pay) coverage as a standard offering, though policyholders may opt out in writing. Med-Pay is a no-fault coverage designed to help pay for medical expenses resulting from a covered auto accident, regardless of who was at fault.
Key points to understand (confirm all details with your insurance provider and a qualified attorney, as coverage varies by policy):
- There is no hard statutory deadline in Colorado law requiring you to seek care within a specific number of days to preserve Med-Pay eligibility — but your policy may contain its own timeliness language.
- Delayed treatment can raise questions from insurers about whether your symptoms are related to the collision. Thorough clinical documentation connecting your symptoms to the accident is important.
- Colorado Med-Pay may help cover eligible medical expenses — including chiropractic care, physical therapy, and diagnostic imaging — depending on your policy limits and terms.
- Coordination with health insurance is possible, but the interaction between Med-Pay, health insurance, and PIP (if applicable) can be complex.
If you’re unsure whether your delayed treatment will be covered, speaking with a provider who understands Colorado Med-Pay laws — and an attorney familiar with Colorado personal injury claims — is the most reliable path to clarity.
How to Prove Delayed Whiplash Symptoms to an Insurance Company
Insurance adjusters are trained to look for gaps in care and documentation. A delayed presentation — even one that is entirely consistent with the known physiology of CAD syndrome — can be used to question the legitimacy of your injury if it isn’t properly documented.
Here is what comprehensive, AMA-guideline-aligned documentation typically includes:
- A detailed clinical narrative connecting your mechanism of injury (the collision) to your specific symptom presentation
- Objective physical examination findings — range of motion measurements, orthopedic test results, neurological screening outcomes
- Advanced imaging reports, where applicable (MRI, DMX), with radiologist or specialist interpretation
- A documented symptom timeline establishing when symptoms appeared and how they have evolved
- Functional impact documentation — how your injury is affecting your daily activities, work capacity, and quality of life
The difference between a clinical record that supports a claim and one that doesn’t often comes down to the specificity and medical-legal fluency of the provider who wrote it. Specialists trained in auto accident biomechanics understand how to structure documentation that meets the evidentiary standards insurance carriers and personal injury attorneys require.
Documentation standards can matter significantly in claims. Talk to your provider and attorney about what’s needed for your specific situation.
Frequently Asked Questions
How long after a car accident can whiplash symptoms appear?
Whiplash symptoms commonly appear within 6–72 hours of a collision, with many patients reporting that pain peaks around the 48–72 hour mark. In some cases, symptoms may not become fully apparent for up to a week, particularly when soft tissue inflammation develops gradually. This delayed presentation is a well-documented physiological response, not a sign that the injury is minor.
Why do whiplash symptoms get worse after a few days?
The primary mechanism is the delayed inflammatory cascade. At the time of impact, adrenaline and cortisol suppress pain perception. As these hormones clear — typically within the first 12–24 hours — the immune system begins releasing pro-inflammatory cytokines to the injured cervical tissues. This inflammatory response produces swelling, nerve irritation, and muscle spasm that typically intensify before they begin to resolve.
Can neuro-inflammation cause brain fog after a rear-end collision?
Research suggests that neurological involvement in cervical trauma — including irritation of upper cervical nerve roots and, in some cases, mild traumatic brain injury — may contribute to cognitive symptoms such as difficulty concentrating, memory disruption, and mental fatigue. The headache and dizziness overlap between whiplash and concussion presentations is clinically significant and worth discussing with a qualified provider. These symptoms should always be evaluated by a licensed clinician.
What is the difference between standard ER X-rays and DMX for whiplash?
Standard X-rays detect fractures and bony abnormalities but cannot image soft tissue structures like ligaments, discs, or muscle. Digital Motion X-Ray (DMX) captures the cervical spine in motion, allowing clinicians to identify ligament laxity — abnormal vertebral movement that indicates structural instability — which static imaging cannot reveal.
What are the AMA guidelines for documenting soft tissue injuries?
The American Medical Association provides guidelines for evaluating and rating impairment from soft tissue injuries, including cervical spine conditions. Compliant documentation typically includes objective physical examination findings, functional assessment, and, where applicable, imaging evidence. Providers adhering to these standards produce records that are more defensible in insurance and legal contexts.
What To Do Next
If you are reading this 24, 48, or 72 hours after a collision — with pain that is getting worse, not better — your instinct to seek answers was the right one.
The biology is clear: delayed symptoms are not a sign that you are overreacting. They are a sign that your body is responding to a real cervical injury that deserves a real clinical evaluation.
Here’s what we recommend:
- Don’t wait for symptoms to resolve on their own. The window for the most effective early intervention is narrow, and untreated soft tissue injuries carry documented risks of chronicity.
- Get a trauma-informed evaluation from a specialist who understands CAD biomechanics, not just general wellness adjustments.
- Start a symptom log today. Write down what you feel, when it started, and how it’s changing. This documentation matters clinically and for any future insurance interaction.
- Understand your Colorado Med-Pay rights before assuming you have no coverage for delayed care.
Connect With a Verified Specialist — Find a Provider Near You
Every provider in our network has been vetted for credentials, clinical experience in auto accident trauma, and familiarity with Colorado Med-Pay and medical-legal documentation standards.
FIND A SPECIALIST →
ENCUENTRA UN ESPECIALISTA →
Recovery from a cervical acceleration-deceleration injury requires more than just a standard adjustment. Let’s make sure you’re getting the right care, properly documented, from day one.
 Neuro-Inflammation, Radiculopathy, and Crash Recovery: What Your Radiating Pain Is Actually Telling You
Neuro-Inflammation, Radiculopathy, and Crash Recovery: What Your Radiating Pain Is Actually Telling You