
Key Takeaways
- Standard ER CT scans are designed to detect life-threatening brain bleeds — not the microscopic, functional brain deficits that cause brain fog, dizziness, and cognitive fatigue after a crash.
- Concussion symptoms commonly appear 24–72 hours after impact, and in some cases, days or weeks later — meaning a same-day “all clear” does not rule out a mild traumatic brain injury (mTBI).
- The biomechanical forces of Cervical Acceleration-Deceleration (whiplash) can create neurological disruption without any visible structural damage on standard imaging.
- Specialized diagnostics and AMA-adherent documentation may be critical to both your physical recovery and your Colorado insurance claim.
You walked out of the emergency room with a clean CT scan and a nurse telling you that you were fine. But days later, you can’t concentrate at work. The lights feel too bright. You’re exhausted by noon. You feel, in your own words, off.
You are not imagining this. And you are not alone.
A missed concussion after a car accident is far more common than most people realize — not because of negligence, but because of the fundamental limitations of emergency medicine. Understanding why your injury may have gone undetected is the first step toward getting the care and documentation you actually need.
Why the ER Likely Didn’t Catch Your Concussion
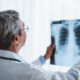
Emergency rooms are designed to save lives. When you arrive after a collision, the clinical priority is ruling out catastrophic, life-threatening conditions: skull fractures, intracranial hemorrhage, and severe structural brain damage. A CT scan does this job well.
What a CT scan does not detect is a mild traumatic brain injury (mTBI) — the clinical term for what most people call a concussion. That’s because a concussion is primarily a functional disruption, not a structural one. The brain’s physical architecture may look completely intact on imaging, while its electrochemical signaling, cellular metabolism, and neurovascular pathways are significantly disrupted at a microscopic level.
Think of it this way: a CT scan can show you a broken bridge. It cannot show you that the traffic lights on that bridge have stopped working.
This distinction — structural vs. functional brain injury — is the single most important concept for anyone who feels symptomatic after a crash but was told their imaging was “normal.” Research published in neurocognitive medicine literature consistently supports that standard neuroimaging has limited sensitivity for detecting the diffuse axonal disruption and neuroinflammatory changes associated with mTBI following motor vehicle collisions.
If you’re in the Denver metro area and were involved in a collision on I-25, I-70, or any of the Front Range’s high-traffic corridors, a post-collision evaluation with a specialist trained in mTBI is a meaningful next step — even if the ER cleared you.
How Cervical Acceleration-Deceleration Creates Brain Trauma Without a “Brain Injury” Diagnosis
The mechanism behind a missed concussion often starts in the neck, not the skull. During a rear-end or frontal collision, the head undergoes rapid Cervical Acceleration-Deceleration — the biomechanical whiplash event where the neck hyperextends and then snaps forward in milliseconds.
During this motion, the brain moves inside the skull. It doesn’t need to strike the skull wall to sustain injury. The shearing forces created by rapid acceleration and deceleration can stretch and disrupt axons — the long, thread-like fibers that neurons use to communicate — throughout the brain’s white matter. This is called diffuse axonal injury, and it does not appear on a standard CT scan.
Simultaneously, the trauma triggers a neuroinflammatory cascade: the brain’s immune cells (microglia) activate, cytokines are released, and cerebral blood flow regulation may be temporarily disrupted. This neuro-inflammation is what drives many of the delayed, persistent symptoms that patients describe as feeling “foggy” or “not themselves” weeks after a crash.
This is also why whiplash and concussion symptoms overlap so significantly — and why treating only the neck pain while ignoring the neurological component often leaves patients stuck in a partial recovery. If you’re experiencing whiplash-related dizziness alongside cognitive symptoms, those two complaints may share a common root cause that warrants a comprehensive evaluation.
Why Symptoms Often Show Up Days (or Weeks) Later
One of the most confusing aspects of a missed concussion is the delay. Many patients feel relatively okay immediately after the crash — adrenaline suppresses pain signals, and the neuroinflammatory response takes time to fully develop. The brain’s initial compensatory mechanisms can mask symptoms for 24 to 72 hours, and in some cases, even longer.
It’s also worth noting that Denver’s high-altitude environment may play a role for some patients. At elevations above 5,000 feet, baseline cerebral oxygen dynamics are already different from sea-level norms. Some clinicians who specialize in post-concussion care have observed that altitude-related factors may exacerbate post-concussion headaches and fatigue in susceptible individuals, though individual responses vary significantly.
The delayed onset of symptoms is clinically recognized and does not make your injury any less real or any less connected to the collision.
Cognitive Symptoms
These are the symptoms most often described as “brain fog” — and they are among the most disorienting because they are invisible to others:
- Difficulty concentrating or staying on task
- Short-term memory gaps (forgetting what you just said, losing words mid-sentence)
- Mental fatigue that arrives much earlier in the day than it used to
- Slowed processing speed — feeling like your thoughts are “buffering”
- Difficulty reading, following conversations, or managing multiple tasks
Vestibular Symptoms
The vestibular system — which governs balance and spatial orientation — is highly sensitive to the biomechanical forces of a crash. Vestibular disruption after mTBI may present as:
- Dizziness or a persistent sense of unsteadiness
- Nausea triggered by motion or visual stimulation (scrolling on a phone, busy environments)
- Sensitivity to light (photophobia) or sound (phonophobia)
- Headaches that worsen with activity or screen time
- Blurred or double vision, or difficulty tracking moving objects
Emotional & Sleep Symptoms
The neuroinflammatory changes associated with mTBI can affect mood regulation and sleep architecture in ways that are often misattributed to stress or anxiety:
- Irritability or emotional reactivity that feels out of character
- Heightened anxiety or a sense of overwhelm
- Depression or emotional flatness
- Difficulty falling asleep or staying asleep
- Sleeping significantly more than usual without feeling rested
If a family member has noticed personality changes, memory lapses, or uncharacteristic behavior in a loved one following a crash, these observations are clinically meaningful. They should be documented and shared with a specialist.
Red Flag Symptoms — When to Seek Urgent Care Immediately
Call 911 or go to the nearest emergency room immediately if you or someone you know experiences any of the following after a car accident:
- Loss of consciousness (even briefly)
- One pupil is larger than the other
- Seizures or convulsions
- Repeated vomiting
- Worsening or severe headache that does not respond to rest
- Slurred speech, weakness, or numbness in limbs
- Inability to recognize people or places
- Extreme confusion or agitation that is escalating
These symptoms may indicate a serious neurological emergency. Do not wait. Do not drive yourself. Call emergency services.
How a Missed Concussion Is Documented for an Insurance Claim in Colorado
For patients navigating a Colorado auto insurance claim — or working with a personal injury attorney — the timing and quality of your medical documentation may matter significantly to your case. Insurance adjusters sometimes challenge delayed-onset injuries precisely because they weren’t diagnosed at the scene or in the ER.
This is where specialized diagnostics and AMA-adherent documentation standards become critical.
Neurocognitive testing for missed concussions — such as computerized cognitive assessments and tools like VITAL CNS — can establish an objective, measurable baseline of cognitive function. Unlike a CT scan, these tools are designed to detect the functional deficits that mTBI causes: processing speed, working memory, reaction time, and executive function. A clinician can use these results to create a documented, defensible record of your cognitive status following the crash.
Advanced imaging tools, including Digital Motion X-Ray (DMX), may also be used to evaluate ligament laxity and cervical instability — soft tissue pathology that is invisible on standard MRIs but may be directly connected to your neurological symptoms. Ligament laxity diagnostics using DMX technology represent a level of clinical specificity that goes well beyond what most emergency rooms or general practitioners can offer.
Colorado’s MedPay (Medical Payments Coverage) may help cover eligible medical expenses for these evaluations, depending on your specific policy. Coverage varies; confirm the details with your insurer and, if applicable, your attorney. Documentation standards can matter significantly in claims — talk to your provider and your legal team about what’s needed to substantiate a delayed-onset mTBI diagnosis.
What Kind of Specialist Should You See After a Missed Concussion?
Not all providers are equally equipped to evaluate, treat, and document a missed concussion following a motor vehicle collision. General practitioners and emergency physicians are trained for acute stabilization — not for the nuanced, multi-system evaluation that post-concussion recovery often requires.
Specialists who may be appropriate for post-crash mTBI evaluation include:
- Chiropractors with advanced training in mTBI and Cervical Acceleration-Deceleration — particularly those who use neurocognitive testing and DMX diagnostics
- Vestibular therapists — for patients whose primary symptoms involve dizziness, balance disruption, or visual tracking difficulties
- Neuropsychologists — for a comprehensive cognitive assessment when symptoms are significantly affecting work or daily function
- Neurologists — when red-flag neurological symptoms are present or escalating
The key is finding a provider who understands both the clinical complexity of post-concussion care and the documentation requirements of a Colorado auto injury claim. Vetted concussion-capable specialists in Denver who work within the medical-legal framework of auto injury recovery represent a meaningfully different level of care than a standard chiropractic adjustment or a follow-up with a general practitioner.
Evidence-based approaches to post-concussion care may help support recovery and function. A licensed clinician can evaluate your specific presentation and determine what is appropriate for your situation.
Don’t Navigate This Alone
Feeling “off” after a crash — but being told you’re fine — is one of the most isolating experiences an accident survivor can have. Your symptoms are real. The science behind why they were missed is well-established. And the path forward exists.
Connect with vetted concussion-capable specialists in Denver who understand both the clinical complexity of a missed mTBI and the documentation standards that matter for your Colorado auto insurance claim.
→ Find a Specialist | Encuentra un Especialista
This page provides general educational information and does not provide medical, legal, or insurance advice. For guidance specific to your situation, consult a licensed healthcare professional and/or a qualified attorney, and confirm coverage details with your insurance provider. If symptoms are severe, worsening, or you are concerned about a head or neck injury, seek urgent or emergency care.
Frequently Asked Questions
Can a hospital ER miss a concussion on a CT scan?
Yes. CT scans are designed to detect structural damage — skull fractures and brain bleeds. A concussion (mild traumatic brain injury) is primarily a functional disruption at the cellular and electrochemical level. Standard CT imaging typically does not detect the microscopic axonal disruption or neuroinflammatory changes associated with mTBI. A normal CT result does not rule out a concussion.
Why do concussion symptoms appear days after a car accident?
The neuroinflammatory cascade triggered by the trauma takes time to develop fully. Adrenaline and the body’s acute stress response can also suppress pain and cognitive symptoms in the immediate aftermath of a crash. Delayed onset of 24–72 hours — or longer — is clinically recognized and does not indicate that the injury is unrelated to the collision.
What is the difference between whiplash brain fog and a concussion?
Whiplash (Cervical Acceleration-Deceleration) and concussion frequently co-occur and share overlapping symptoms, including brain fog, dizziness, and headaches. Whiplash primarily involves soft tissue and cervical spine injury; a concussion involves neurological disruption. In many car accident cases, both are present simultaneously. A specialist evaluation can help differentiate and address both components.
How do you prove a concussion if it wasn’t diagnosed immediately?
Neurocognitive testing, vestibular assessments, and advanced imaging tools like DMX can establish objective, measurable evidence of functional deficits and soft tissue pathology. AMA-adherent documentation from a qualified specialist creates a defensible clinical record connecting your current symptoms to the collision. An attorney familiar with Colorado auto injury claims can advise on the legal evidentiary standards.
What kind of doctor treats a delayed concussion after a car accident?
Depending on your symptoms, appropriate specialists may include mTBI-trained chiropractors, vestibular therapists, neuropsychologists, or neurologists. The most important factor is finding a provider with specific experience in post-collision mTBI evaluation and medical-legal documentation — not simply a provider who treats general headaches or neck pain.
Does Colorado Med-Pay cover treatments for delayed concussions?
Colorado MedPay may help cover eligible medical expenses depending on your individual policy. Coverage terms vary significantly. Confirm the details with your insurance provider and, if applicable, a qualified personal injury attorney before assuming coverage.
How long do I have to report a delayed concussion to my auto insurance?
Colorado’s statute of limitations for personal injury claims is generally three years from the date of the accident, but specific reporting requirements and deadlines vary by insurer and policy. Consult a qualified Colorado personal injury attorney for guidance specific to your situation. Do not delay seeking care while waiting for legal clarity — early documentation supports your claim.

 DMX vs. MRI vs. X-Ray for Crash Injuries: What Each Scan Actually Shows (And Why It Matters for Your Claim)
DMX vs. MRI vs. X-Ray for Crash Injuries: What Each Scan Actually Shows (And Why It Matters for Your Claim)